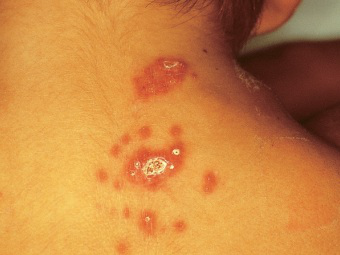
Most cases of tularemia are char- acter Led by the formation of a focal ulcer at the site of entry of the causative bacillus, enlargement of regional lymph nodes, and a constitutional reaction of fever, prostration, myalgia, and headache. There may be pneumonia, which is occasionally accompanied by pleurisy or a typhoid-like illness.
Francisella tularensis, the microbial agent, is transmitted to humans by insect vectors such as ticks or .deer flies, by the handling or ingestion of infected animal tissues, or by inhalation of infected aerosols. The clinical diagnosis is confirmed by demonstration of bacteremia, by isolation of the bacillus from the sputum, tissue exudates, or gastric washings, and by demonstration of serum agglutinins in early convalescence.
Historical Features.
The knowledge of the ecology and clinical features of tularemia has been developed in the United States through the pioneering work of Francis and other Public Health Service investigators. McCoy described the disease in 1911 while studying a plague like illness in ground squirrels in Tulare County, California. The first clinical description and bacteriologic proof of illness is attributed to Wherry and Lamb in 1914. In a series of studies conducted in Utah and elsewhere, Francis (1928) incriminated rabbits as important animal hosts and established the transmissibility of disease by deer flies.
Etiology, Specific Laboratory Diagnosis, and Epidemiology.
Tularemia is of considerable interest because the causative micro-organism is a member of the important gram-negative group characterized by intracellular parasitism about which basic information on immunity mechanisms is incomplete. The bacillus’ is pleomorphic and non- motile, and propagates best on such artificial media as blood-glucose-cysteine agar or following inoculation of animals with suspensions of infected tissues.
Culture.
During the early stages of illness, F. tularensis is isolated readily by direct culture in appropriate media or by the subcutaneous or intraperitoneal inoculation of exudate into mice or guinea pigs. Positive cultures are obtained from the local ulcer or regional lymph nodes during the first several weeks in patients with ulceroglandular type of illness. Regardless of the clinical type of tularemia, viable organisms may be isolated from nasopharyngeal or gastric washings during the active systemic phases of illness. Pleural fluid and bronchial secretions are suitable for cultural purposes. Bacteremia may be demonstrated in all forms, although isolation from the blood by culture on an artificial medium is difficult because of the paucity of organisms present.
Organisms have been isolated from cerebrospinal fluid or bone marrow, although such cultural procedures are rarely indicated. Under ideal conditions, if suitable media are inoculated with appropriate material, the organism may be identified within two to four days. Impression smears of splenic tissues often reveal the characteristic coccal or bacillary forms intracellularly following preparation with Giemsa or Way son’s plague stain.
Serologic Diagnosis.
The conventional serum agglutination reaction is a very useful diagnostic test, because specific agglutinins appear within eight to ten days from the onset of illness. Maximal titers are reached in about four weeks. Demonstration of a rise in titer through examination of serial specimens is confirmatory evidence of infection, although single titers of 1:160 or more are usually significant. Sera from patients with brucellosis or tularemia may show cross-agglutination, although the titer is usually higher with the homologous antigen.
Cutaneous Test.
Foshay described a diagnostic skin test that consists of the intradermal inoculation of a purified antigen consisting of a killed suspension of F. tularensis. The reaction is of the delayed tuberculin-type, becoming positive in 48 hours. The test is highly specific and becomes positive during the first week of tularemia either prior to or coincident with the development of agglutinins. The test remains positive for years.
Epidemiology.
Tularemia has been detected in many countries of the Northern Hemisphere. F. tularensis has been found in practically all animal species. In much of North America cottontail rabbits are the most important animal host and were formerly a very common source of the ulcero- glandular and typhoidal forms of tularemia. Restricted sale of wild rabbits in metropolitan areas resulted in a sharp decline of the disease.
The clinical infection develops following puncture wounds by bony spicules of infected rabbits or by the ingestion of improperly cooked food. Foxes, squirrels, rats, mice —indeed, all rodents — have been incriminated as sources of infection. Streams are contaminated for variable periods by infected animal carcasses (or by other less well understood routes), so that drinking the water or handling aquatic mammals such as muskrats may be hazardous.
Many cases have their origin from infected arthropods such as ticks, deer flies, or mosquitoes. In North America the ticks Dermacentor andersoni, Dermacentor variabilis, and the Lone Star tick are important reservoirs and vectors. Infected female ticks transmit F. tularensis transovarially. A primary ulcer often forms at the site of tick attachment.
Tularemia occurs in all seasons: among hunters and trappers in the fall and winter, and during the spring and summer when ticks and deer flies are active. All ages and both sexes are susceptible.
Mechanism of Infection and Pathology.
The disease may present in a variety of forms with two major subdivisions, depending on whether or not the initial site of entry can be visualized. In all forms there is lymph node involvement. In most instances there is a primary ulcer, variable in size, which may be located on the skin (ulcero- glandular), in the eye (oculoglandular), or in the nasopharynx with necrotizing lesions. Sometimes the cutaneous lesion may be insignificant, so that the picture is that of “glandular tularemia” without an overt primary lesion. The entry also may be through the intestinal tract (enteric or typhoidal) or via the lungs (pulmonary).
Following infection, F. tularensis reaches the blood via the lymphatics and nodes; the microbe, although phagocytized, resides intracellularly without loss of viability. Granulomatous lesions develop within the reticuloendothelial system, particularly in lymph nodes, liver, and .spleen. These lesions, usually hyperplastic, bear some resemblance to tuberculosis and may caseate or form small local abscesses. The macrophage is the predominant cell type that surrounds an area of caseous necrosis. Langhans’ cells are observed occasionally, and the larger lesions are liable to central abscess formation.
Bronchopneumonia is a common development in tularemia, occurring in approximately 30 per cent of patients who acquire the disease, regardless of the type of infection. Histologically, the early lesion is edematous, and consists of fibrin and leukocytes associated with necrosis of alveo
lar walls. In non-necrotic areas the exudate consists of the large mononuclear type. The gross lesions resemble the bronchopneumonia of tuberculosis,’ although histologically there is less epithelioid cell transformation. Tubercle-like nodules are more common in lymph nodes than in the lungs. Mediastinal nodes are involved frequently.
Clinical Manifestations.
The incubation period of tularemia ranges from two to ten days. Headache, fever, and toxic signs characterize all forms of the illness and are in no way dissimilar to those in other infectious illnesses. The pertinent historic and epidemiologic features are often helpful clues, and in approximately three fourths of all patients there is a primary lesion associated with adenopathy.
Ulceroglandular Tularemia.
The initial lesion begins as a reddish papule, which is often undermined and more extensive than the small area of superficial induration indicates. Neighboring and draining lymph nodes are enlarged, tender, and discrete. Fluctuation of these nodes occurs later in the illness, after two or more weeks, when other acute signs may have partially abated. Such diseased nodes may subsequently require incision and drainage. The lymph nodes during the early stages are laden with F. tularensis and, if incised, may provoke bacteremia and toxemia. Fluctuant buboes four or more weeks old are usually sterile. Generalized lymphadenopathy occurs. Systemic signs of toxemia may be severe in ulceroglandular tularemia, although most cases are mild or moderate in severity. Pneumonia of all gradations may accompany this type of infection.
Enteric Form of Tularemia (Typhoidal or Cryptogenic).
Following ingestion of infected animal tissues or water, ulcerative lesions of the buccal mucosa, pharynx, and intestine, and subsequent involvement of cervical, pharyngeal, and mesenteric lymph nodes may occur. The course of illness may be fulminant and fatal unless the disease is recognized and treated properly. Certain of these patients manifest illness that is similar to various forms of gastroenteritis and typhoid fever. These patients may be severely ill with sustained high fever, profound toxicity, stupor, and delirium or coma. This typhoidal systemic reaction may typify any of the clinical varieties of tularemia regardless of the presence of a cutaneous lesion. The term “cryptogenic” has often been used to connote the absence of an obvious portal of entry.
What IS Pulmonary Tularemia.
Lung involvement occurs in all forms of tularemia, subsequent to the bacteremia. Available evidence suggests that primary tularemia pneumonia is an entity, particularly in those persons such as laboratory workers who are exposed to infected aerosols. The incubation period varies from two to five days, depending upon the number of viable bacteria inhaled. In addition to headache, fever, malaise, and prostration, there is a nonproductive harassing cough and a sensation of substernal discomfort. Later the sputum may be mucoid or bloody and, in severely ill patients, there are pleural pain, dyspnea, tachycardia, and cyanosis.
In spite of extensive pulmonary involvement, there may be a paucity of physical signs. The early roentgenographic signs, seldom evident before the second to the fourth day of fever, consist of small irregular oval lesions with hilar adenopathy. Later in the illness, the infiltrate may be annular. True abscess formation is rare, although during resolution and convalescence, which in untreated cases or in those treated late may be prolonged, shadows suggesting abscess formation may be noted. Pleuritis with effusion is not uncommon.
Oculoglandular Tularemia.
Following ocular contamination there may be pain, photophobia, intense congestion, itching, lacrimation, chemosis, and a mucopurulent discharge. Small yellowish granulomatous lesions may appear on the palpebral conjunctiva or cornea and may eventually ulcerate. The preauricular and other regional lymph nodes may enlarge and ultimately suppurate. In untreated patients, serious ocular complications including corneal perforation or optic atrophy may ensue.
Other General Manifestations.
Initially, in severely ill patients, there is a rigor followed by pyrexia that persists for a month or more. The fever may be continuously high or remittent, and defervescence is usually gradual. Hepatomegaly and splenomegaly with tenderness over the respective organs are relatively common. Toxic signs in all cases include fever, headache, myalgia, and nausea. Hashes mOTS MV,’Nteu Present,
they consist of localized papular lesions along the peripheral lymphatics or maculopapular body eruptions. In untreated patients or in those first giyen antimicrobial therapy late in the course of illness, convalescence may be prolonged with sporadic episodes of fever, weakness, muscular pains, and chronic respiratory signs.
Nonspecific Laboratory Findings. The erythrocyte sedimentation rate and C-reactive protein are elevated during the active stages. In contrast, the total blood leukocyte count is usually normal or low. Occasionally there may be moderate leukocytosis. Mild albuminuria may occur at the height of illness.
Differential Diagnosis.
Ulceroglandular tularemia is recognized readily in endemic areas. Punctate lesions with surrounding erythema at the site of prior arthropod attachment suggest Rocky Mountain spotted fever, particularly when associated with fever, headache, and toxic signs. The absence of a rash would favor tularemia, because patients with rickettsial disease develop a characteristic exanthem. Meningococcemia is recognized by its fulminant character, the typical exanthem, leukocytosis, and the bacteriologic findings. Fever, toxic signs, pharyngitis, adenitis, hepatomegaly, and splenomegaly are common to tularemia and infectious mononucleosis.