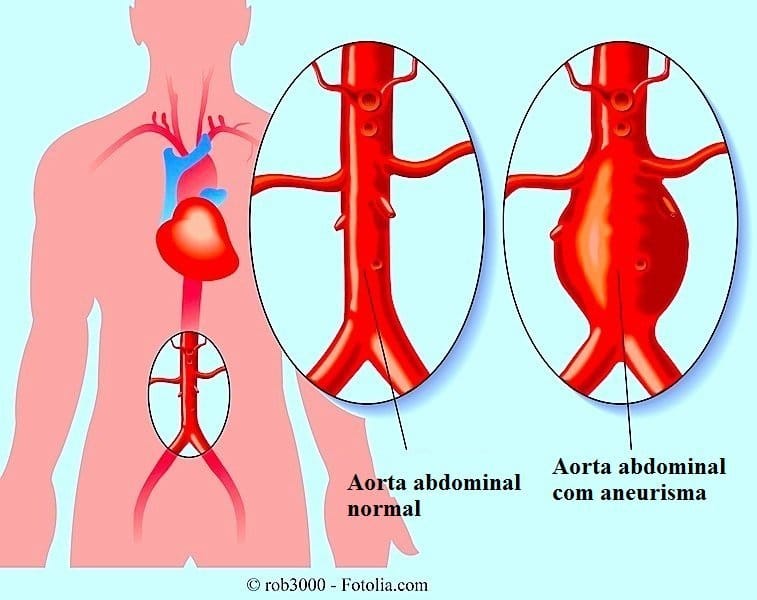
Dissecting aneurysm of the aorta is also called aortic dissection of the aorta. According to Wolfe and Moran, there are at least 2000 new cases of dissecting aneurysm each year in the United States. The disease tends to occur in certain settings. It is most common in men of middle age with hypertension, but is also found in Marfan’s syndrome, cystic medial necrosis, or coarctation of the aorta and seems more common in pregnancy. The relationship of dissecting aneurysm to pregnancy is discussed in a recent article (Am J Med, 1983). Dissecting aneurysm may occur in certain heritable disorders of connective tissue, including Ehlers-Danlos syndrome, and has been described as a complication of relapsing polychondritis. The prevalence of aortic dissection is increased in patients with bicuspid aortic valves.
Ordinanly the dissection begins with an aortic intimal tear, followed by a dissecting channel in the media, followed by reentry from the intima back into the aortic lumen or rupture through the adventitia. Thus a double-barreled aorta may be produced. Approximately 50 per cent of aortic dissections begin in the ascending aorta, 30 per cent in the aortic arch, and 20 per cent in the descending aorta. Dissecting aneurysm may be related to frauma, especially that produced by an angiographic catheter or aortic balloon catheter striking an arteriosclerotic plaque in the aorta.
Aortocoronary bypass grafting may be complicated by dissecting aneurysm. A dissecting aneurysm may extend proximally to the aortic valve area, thus causing aortic valvular insufficiency; it may surround the coronary arteries, producing myocardial infarction; it may extend along the carotid sheath to cause hemiplegia. It may involve the blood supply to the spinal cord, leading to paraplegia and anesthesia below the level of involvement. It may involve the renal artery, thus aggravating pre-existing arterial hypertension. Hypertension may also be aggravated by carotid artery involvement when it interferes with the carotid sinus barore-ceptor response. Rupture into the pericardium may lead to cardiac tamponade and rapid demise.
PROGNOSIS of Dissecting aneurysm In Aorta
The prognosis is poor in aortic dissecting aneurysm. If untreated, approximately 20 per cent of patients die within 24 hours and 37 per cent in 48 hours. A small percentage of patients, probably less than 10 per cent, live for a year and may survive with chronic or even severe aortic insufficiency. Rarely, a dissection in the descending aorta may re-enter the original lumen, producing a double-barreled aorta, which may allow survival for years. With surgical resection of the diseased segment and aortic graft replacement, as many as 75 per cent may survive. At Stanford, the operative mortality was 29 per cent in 125 patients. Of those who survived operation, 76 per cent lived five years or more (Miller et al.). The prognosis is better for either medical or surgical treatment when the dissection begins distal to the aortic arch. In this group, 50 per cent may survive the first three weeks even without modern therapy.
TREATMENT of Dissecting aneurysm In Aorta
Treatment may be either surgical or medical Surgical management usually consists of resection of the involved segment and replacement with a prosthetic graft. Operative management is especially to be considered in the following circumstances: (1) when there is leaking from the dissection, which most commonly takes place into the left hemithorax or pencardium; (2) when the ascending aorta or arch is involved; (3) when the cerebral circulation is compromised but not to a degree incompatible with recovery; (4) with severe heart failure caused by aortic regurgitation; (5) when there is evidence of continued dissection; (6) when pain and blood pressure cannot be controlled; and (7) when hypertension is absent.
Initial medical management is suggested when the process is limited to the descending aorta, except when there is continued pain, evidence of bleeding, or extension of the dissection. Medical management involves contTol of hypertension and administration of drugs to lessen the systolic ejection force of the heart. Hypertension is treated with trimethaphan (Arfonad) or with oral or intravenous alpha methyidopa. Wolfe and Moran favor intravenous sodium nitroprusside as the initial agent. The systolic blood pressure is reduced to 100 to 120 mm Hg. Along with these antihypertensive agents, oral propranolol, 10 to 40 mg four times daily, is given to reduce the velocity of left ventricular ejection. In one series, 17 of 33 patients treated medically survived, and in another, 10 of 12. In the Peter Bent Bngham Hospital senes, 26 of 31 patients with aortic dissection had contraindications to medical therapy; 17 of 22 did well after surgical correction. When dissection was limited to the descending aorta, none of 14 patients had contraindications to medical therapy, which was successful in each instance.
Medical management may be considered when the process is more than two weeks old. Resection of the dissected area, followed by grafting, may be done later when the condition of the patient is stabilized. Progressive enlargement of the aneurysm is an indication for surgical repair in patients who have received medical therapy. The majority can be brought through the acute phase of the illness alive. However, the long-term outlook in medically treated patients is uncertain, and many will do better with surgical treatment once the condition has stabilized. Long-term antihypertensive therapy should be considered, if indicated.