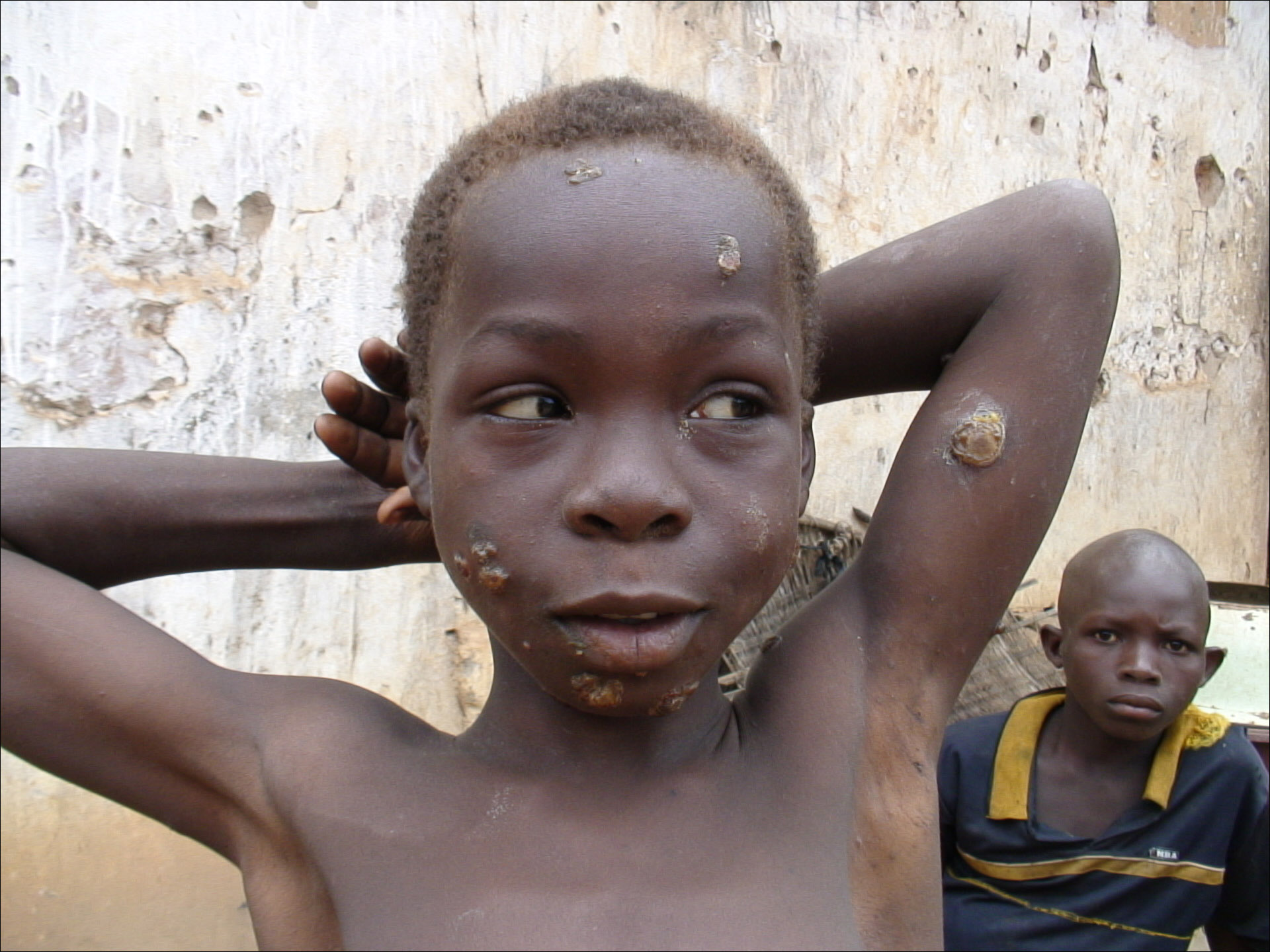
Yaws diseases is produced by a spirochetal microorganism, T. pertenue, which causes a chronic human infection, most often with onset in childhood. An initial cutaneous lesion usually appears, followed by relapsing infectious secondary nondestructive lesions of the skin, periosteum, and bones, frequently interspersed with symptom-free periods. Late manifestations include destructive and deforming lesions of skin, bones, and joints. Hyperkeratosis, notably of the soles, may develop in secondary and late yaws. There is no evidence of cardiac or nervous system involvement or of prenatal manifestations. Infected persons slowly develop relative immunity, and humoral antibodies can be detected by serologic tests reactive also in other treponematoses (syphilis, pinta).
History of Yaws Diseases.
Yaws probably existed in Africa from remote times. Early accounts suggest that it was brought to the West Indies with the slave trade in the sixteenth century. By the eighteenth century it had become a serious health problem of the Antilles, Central America, and South America, as well as in areas of Oceania and Southeast Asia. Sauvages (1778) proposed the name frambesia for the disease because of the raspberry-like appearance of its papillomatous secondary lesions. Moseley (1800) observed its clinical course, notably that yaws ends in shocking nodes and destructive lesions.
Maxwell (1839) determined its incubation period to be three to four weeks following inoculation of lesion material into humans. Castellani (1905) identified T. pertenue as the causative micro-organism of yaws. Lambert (1923) first attempted community-wide treatment with arseni-cals in the Pacific Isles. The advent of long-acting penicillin preparations and single injection therapy revolutionized case treatment and made possible important reduction of yaws by mass penicillin campaigns (World Health Organization, 1950-1970) in the tropics.
Etiology of Yaws Diseases.
The causative agent, T. pertenue, is a helical cell 8 to 12 ^ in length, about 0.2 /x in diameter, with several closely set spirals. It resembles T. pallidum (syphilis) and T. carateum (pinta) morphologically in dark-field illumination and structurally in electron microphotographs. T. pertenue has not been grown in vitro, but will survive for several days without multiplication in The author wishes to acknowledge the valuable advice, criticisms, and suggestions by his colleague Dr. J. Ridet, Medical Officer, Communicable Diseases Division, World Health Organization, Geneva, concerning this article.
Strains stored in glycerin remain virulent for many years at —70° C. (C02 ice) or lower temperatures, e.g., liquid nitrogen or helium. T. pertenue is pathogenic for the same animal species as T. pallidum. The latter causes subclinical “silent” infection in the hamster, whereas T. pertenue causes a specific dermatitis — a procedure sometimes used to differentiate between treponemes in the laboratory (Vaisman, 1969). Pathogenic treponemes closely resembling or identical with T. pertenue have been isolated from wild cynomolgus African monkeys (Fribourg-Blanc et al.; Sepetjian et al., 1968).
Epidemiology and Pathogenesis of Yaws Diseases.
Despite mass penicillin campaigns in recent years, yaws has remained a disease of many rural communities in the intertropical zone in Africa, the Americas, Southeast Asia, and Oceania. Areas of high prevalence of active yaws sometimes lie within a few miles of communities where the disease is rarely observed, depending on the ecologic situation, the evolutionary stage of endemicity, and the number of susceptibles at any given time. There is also a higher frequency of early yaws lesions in the rainy than in the dry season (Harding, 1947).
Moreover, skin lesions are less frequent in cooler climates in mountainous tropical communities where they also become less moist and where papillomas tend to erupt in sweaty, mucocutaneous junctions and skin folds rather than involving the flat body surfaces (Ramsey, 1925). Furthermore, the occasional yaws lesions encountered following mass penicillin campaigns appear to be less extensive and less moist. In areas where no further lesions are encountered following such campaigns, continued specific seroreactivity (TPI) in a small proportion of children born after the campaigns has suggested the possibility of asymptomatic infection taking place in the new circumstances.
T. pertenue is incapable of penetrating unbroken skin. It is also unable to pass the placenta and cause congenital yaws. Transmission usually occurs through contact of skin abrasions, cuts, or lesions, e.g., trauma, injury, dermatoses, with infectious yaws lesions of another person. Indirect transmission via contaminated hands is believed to occur among children. Nursing mothers are sometimes infected directly by their infants.
In addition to early infectious lesions, untreated latent yaws cases —which are liable to relapse with active lesions —form an important part of the reservoir maintaining the disease in rural communities. Humidity, moisture-holding soil, and mean annual temperatures of 27° C. or more are also necessary for the spread of yaws. Moreover, transmission is favored by scant clothing, bare feet, crowded dwellings, and deficient personal hygiene. The gradual improvement of environmental and socioeconomic conditions will reduce the attack rate of yaws (Saxena and Prasad, 1963).
No true vector has been found in which T. pertenue actually multiplies, but it has been shown that disease can be transmitted by experimentally infected gnats. In some areas Hippelates pallipes may serve as mechanical carriers (Kumm and Tur-ner, 1936). Geographic coexistence of foci of human yaws and natural treponematoses of wild cynomolgus monkeys have been observed in Africa (Baylet et al., 1970).
The age distribution of yaws depends on the rate of transmission and level of endemicity. In hyperendemic communities, e.g., the former Netherlands New Guinea (Kranendonk), the highest relative frequency of infectious lesions was in the two- to five-year-olds, with a seroprevalence of more than 90 per cent at an early age, pointing to almost complete epidemic “saturation” of the community with yaws. In areas of moderate or low endemicity the highest seroprevalence is in older age groups.
Following mass penicillin campaigns, maximal seroprevalence was in the 45- to 59-year-olds, e.g., Nigeria, signaling regression of a hyperendemic situation many years ago. In the latter instance many more young individuals are susceptible to yaws in the new generation, but there are also more barriers to impede renewed spread of the infection, e.g., education, health consciousness, chemotherapy, and health services. However, the greater number of serologically nonreactive young people in the new generation have, when reaching puberty, less protective cross immunity to infection with venereal syphilis. This has been reported to be among the reasons for the increased incidence of syphilis noted in tropical countries in the last decade.
Pathology of Yaws Diseases
A main pathologic feature of yaws is the involvement of the skin. In early lesions the epidermis is thickened. There are cell infiltration (“plasmacytoma”) of the dermis, hyperplasia, edema, and the presence of many treponemes. The papillae are elongated, often with thickening of the interpapillary pegs. Proliferation of vascular endothelium and obstruction of vessels are less characteristic of yaws than of syphilis. The epithelium may show hyperkeratosis, become superficially eroded, and be covered by dried exudate.
The acanthotic epidermis and the papillary proliferation give rise to a fungating, frambes form, crust-covered lesion. Diffuse periostitis and cortical rarefaction of the long bones are common in early yaws and are more marked than in venereal syphilis. The late lesions of yaws are due to a different tissue response, and endarteritis is observed histopathologically. Late lesions include ulcerating granulomatous nodules and gumma of the skin and bones. The gumma is built of elements similar to syphilitic lesions. Late skeletal affliction is mostly characterized by periosteal proliferation, rarefaction, or destruction of multiple areas of the long bones which can lead to extensive deformities.
Clinical Characteristics of Yaws Diseases.
At the site of entry of T. pertenue an initial lesion usually develops after an incubation period of three to four weeks. The implantation is facilitated by previous breaks in the skin (abrasion, injury, vaccination). The lesion is a papule situated on the legs in more than half the cases. In babies and toddlers it often appears on the buttocks or in the perineum. The papule grows into a round, broad-based granulomatous lesion (“mother yaw”) covered by a serous crust from which T. pertenue can be recovered. The regional lymph nodes are frequently enlarged, not “shotty,” and do not suppurate. An initial lesion will heal spontaneously within three to six months; ulcerating initial lesions require more time to heal.
As a result of early treponemia a generalized secondary eruption appears before or after the healing of the initial lesion. The most frequent and characteristic eruptions are roundish, raised, rough, granulomatous papules (“yaws” or fram-besides), often covered by a brownish crust. These lesions appear anywhere on the skin, but rarely on the scalp. They sometimes show arciform arrangements. Secondary lesions may last for more than six months. A new crop may appear before the preceding lesions heal. Relapsing crops tend increasingly to become localized, e.g., to peri axillary, perianal, or circumoral areas. Sometimes the papilloma may be solitary.
Plantar papules appear late, often after the generalized eruption, and are modified by the thick keratotic layer characteristic of barefoot people: a cherry-like granuloma appears in a well of cracked horny layer, frequently giving rise to painful disability (“crab yaws”). On the body, micropapular as well as various forms of macular or desquamative macular (“pian dartre”) lesions may also appear. Lesions of mucous membranes are rare, but occur. Desqua-matous macules can develop in the palms and notably on the soles, which are sometimes covered by a thick hyperkeratotic layer. In addition to skin eruptions in early yaws, there is superficial lymph node enlargement. In many cases there are pain and tenderness of the tibial shaft and other long bones owing to early periostitis. Such periostitis sometimes leads to saber tibia and polydactylus. In many cases the general health of the patient appears little affected; in others there are systemic manifestations, with irregular fever, loss of appetite, and weight loss.
The secondary lesions begin to regress after several months, but relapses may occur on and off for four to five years before true latency is reached. The latter can be interrupted by late lesions of several types. (1) Superficial ulcerations of the skin with central healing tendency are observed, and cutaneous and subcutaneous nodules with ulceration and marginal healing may leave markedly depigmented atrophic scars, sometimes with deforming contractures. (2) Diffuse or more localized hyperkeratosis of the soles — less frequently of the palms —with Assuring and pitting can result in a characteristic mottled pattern, occasionally complicated by ulceration and sometimes developing more than 15 years after the infection. (3) Ostial or periosteal gummatous lesions of the tibia and other long bones may penetrate subcutaneous and cutaneous tissues, resulting in chronic ulcerations. These may also affect tarsal and carpal bones, the scapula, the sternum, and the skull. Affliction of palatal nasal structures may lead to gangosa (rhinopharyngitis mutilans), a spectacular condition similar to that in syphilis. The osteitis and periostitis can occur both in associationciation with generalized skin lesions and after these have receded.
Other yaws lesions are less common and include painless subcutaneous fibromatous juxta-articular nodes, paranasal egg-shaped swelling of the superior maxillary bone (goundou), chronic late macular or hyperkeratotic lesions of palmar surfaces, and volar aspects of wrists and insteps of soles, frequently followed by depigmentation.
Diagnosis of Yaws Diseases.
Typical early yaws lesions are generally not confused clinically with other conditions. Ulcerated initial leg lesions may sometimes be mistaken for other ulcerations, e.g., tropical ulcer. Also, spirochetes found in tropical ulcers resembling Borrelia vincentii may be mistaken for T. pertenue. Facial yaws papules may look like crusted impetigo. Individual lesions may resemble those of secondary syphilis or cutaneous leishmaniasis. Demonstration of treponemes by microscopic dark-field examination of exudate from the lesion and seroreactivity in reagin and treponemal antibody tests (VDRL, FTA, TPI) serve to distinguish yaws from other conditions except those of the treponematosis group. Reagin tests become positive in serum about a month after the initial lesion i Li and Soebekti. 1955 \ and TPI titers can be very high 1:2560 > in early yaws WHO, Eastern Nigeria, 1968). Ulcerating contractures and mutilating lesions may present differential diagnostic problems in relation notably to leprosy and tuberculosis. Hyperkeratosis of the soles is often confused with other plantar conditions, mainly keratoma plantare sulcatum, plantar pitting, and tropical hyperkeratotic conditions of unknown origin (Hackett and Lowenthal).
Prognosis of Yaws Diseases.
In infected persons the prognosis is favorable when early treatment is provided. Otherwise, periodic infectious recurrences over many years give rise to months of partial incapacity. An undetermined number of infected persons develop late lesions. Others go on to spontaneous clinical cure; some also become serologically non-reactive (“burnt-out yaws”). Among those developing late chronic lesions extensive incapacitation and deformities often result.
Treatment and Control. The aim of treatment of individual patients is cure of the early disease and prevention of late manifestations. Intramuscular injection of 1.2 mega units of benzathine penicillin or 2.4 megaunits of PAM (procaine penicillin G in oil and 2 per cent monostearate) in adults and half doses for children suffices to cause disappearance of early lesions and prevent relapses. The response is dramatic. The early lesions usually become dark-field-negative within 48 hours, and healing takes place within 1 to 2 weeks. Serologic titers decline, but many retain low-titer reagin seroreactivity, depending on the duration of the infection (D’Mello and Krag, 1955).
Penicillin sometimes causes a Herxheimer reaction. The usual safeguards against hypersensitivity reactions to penicillin should be taken (see Syphilis). Persons with late yaws lesions may require repeated therapy. Oxytetracycline and chlortetracycline are reported to be useful in cases of deforming osteoperiostitis, indolent gummas, or ulcerations. Two grams daily for five to ten days in adults and proportionately less for children are given. Ulcerations of late yaws may also require application of local antiseptic dressings. Deformities caused by chronic osteitis and contractures necessitate local surgery at times in addition to drug therapy.
In the efforts to achieve community-wide control of yaws, the previous work of the Jamaica Yaws Commission 115361 was in recent years extended under the auspices of the World Health Organization. Since 1950 some 200 million people in 45 countries were examined, and some 50 million treated with long-acting penicillin in large-scale control programs. The aim was (1) to survey entire area populations so as to control the reservoir of infection, (2) to interrupt the spread of yaws through mass, treatment, rendering early cases noncontagious, preventing infectious recurrences, and aborting incubating disease, and (3) to undertake post-campaign yaws surveillance by periodic re-surveys to detect and promptly treat overlooked cases or new infections that might arise.
Untreated early cases free of clinical symptoms between outbreaks form an important part of the reservoir of infection and contribute to maintain the disease in rural communities. Accordingly, mass treatment criteria in these campaigns were based on a certain association in the population between the occurrence of clinically active lesions and of seroprevalence owing both to such lesions and to clinically symptom-free infections (Hackett and Guthe, 1956).
These criteria for mass treatment are: (1) When the prevalence of active yaws cases is 10 per cent or higher (hyperendemic areas), more than 50 per cent of the population is seroreactive, and all members of the community are to be treated. (2) When there are 5 to 10 per cent of active cases (mesoendemic area), all children and their obvious contacts are treated, as most contagious cases occur in the lower age groups. (3) When there are less than 5 per cent active cases (hypoendemic areas), solely case and contact treatment is provided. This wide use of penicillin results in rapid regression of active lesions. The prevalence thus has declined within a few years from more than 20 per cent to less than 1 per cent following mass campaigns in many areas.
Prophylaxis of Yaws Diseases.
Prevention, of yaws depends on avoidance of minor injuries to the skin, and of shielding of open wounds and abrasions from contamination by flies. Open infectious lesions should be protected. Health education should aim at improvement of personal hygiene (soap) and community hygiene (water). Children with infectious lesions should be treated and excluded from school until noninfectious. Mass therapy represents an important control measure. No method of artificial immunization is available.