Table of Contents
ToggleBrief reminder on what Candida is
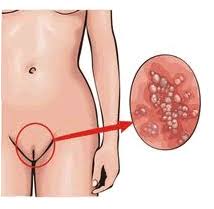
The candida (or candidiasis ) is a fungal infection (or mycosis ) caused by the fungus Candida albicans .
Scientific classification of Candida albicans
Candida albicans is a saprophytic mushroom (that is, which feeds on rotting material), belonging to the saccharomycetes family . Saccharomycetes are particular single-celled organisms that live in colonies and fall into the category of so-called yeasts (exactly like Saccharomyces cerevisiae , the yeast used for bread ).
Causes
What are the Causes of Vaginal Candida?
Vaginal candida arises when the defense mechanisms responsible for controlling the proliferation of Candida albicans in the female genitalia are no longer present.Remember that Candida albicans is harmless to the human body, as long as the immune system of the latter is able to control its proliferation.
Favoring Factors the Vaginal Candidiasis
Several factors can compromise the efficiency of the defense mechanisms responsible for controlling the proliferation of Candida albicans at the level of the female genitalia and contribute to the development of vaginal candida; among these factors, the most important are:
- Misuse of antibiotics . The use of antibiotics involves the depletion of that part of bacterial flora responsible for regulating the proliferation of microorganisms such as Candida albicans ;
- Bad personal hygiene . The rough drying of the vagina after a shower or a bath creates a humid and warm habitat, ideal for the proliferation of the fungus Candida albicans ;
- Use of poor quality intimate cleaners . Poor quality soaps and shower gels can irritate the vagina and promote fungal multiplication;
- Suffering from immunosuppression . Those suffering from immunosuppression have an inefficient immune system and are therefore predisposed to infections.
Generally, immunosuppression is a typical problem of: people with diseases such as AIDS (which undermine the integrity of the immune system), those taking immunosuppressant drugs (i.e. drugs that lower the immune system ) and the elderly (for reasons physiological); - Suffering from diabetes mellitus . In diabetic individuals , the high amount of glucose in the blood (high blood sugar) favors the multiplication of the fungus Candida albicans , as it represents, for the latter, an almost inexhaustible source of nourishment;
- Pregnancy . The characteristic increase in estrogen observed during pregnancy predisposes pregnant women to Candida albicans infection .
- Sexual intercourse with an infected person . The woman who has sex with a man with candida can develop the same infection, as she is exposed to an important colony of Candida albicans ;
- Share the use of towels , underwear or soaps with an infected person ( mixed use of infected objects ). In these circumstances, what is reported on the occasion of sexual relations with people with candida is repeated.
Is Vaginal Candida a Sexually Transmitted Disease?
According to the medical community, although it may arise from sexual intercourse with affected people, vaginal candida is not to be considered a sexually transmitted disease (such as syphilis or genital herpes ).
Epidemiology
Vaginal candida is a very common infection; in this regard, the statistics say that:
- The vaginal candida figure, together with the bacterial vaginosis and vaginitis from Trichomonas , the list of the first 3 vaginal infections most prevalent in the female population;
- Annually, vaginal candida is a problem for about 20% of the female population;
- Vaginal candida affects approximately 75% of women at least once in their lifetime.
Vaginal thrush is more common among women in antibiotic therapy , women with diabetes mellitus or AIDS, and women taking chemotherapy for the treatment of cancer .
Symptoms and Complications
What are the symptoms of Candida Vaginale?
Typical symptoms and signs of vaginal candida are:
- Pain and itching at the vulva (entrance of the vagina);
- Pain or discomfort during sexual intercourse ( dyspareunia );
- Stinging pain or burning when urinating ( dysuria )
- Fluid leaking from the vagina. Typically, this liquid is odorless, white and sometimes aqueous, sometimes thick.
Furthermore, if the vaginal candida also involves an inflammation of the genital area, the symptomatic picture is enriched with further manifestations, such as:
- Redness of the vulva and vagina;
- Vaginal fissures ;
- Local swelling;
- Very painful skin sores (it is a disorder very rarely observed).
Complications of Vaginal Candida
For some women, vaginal candida represents a relapsing / recurring condition , that is, it occurs from time to time; this situation is not serious from a clinical point of view, but it can have some repercussions on the quality of the patient’s sexual life.
Furthermore, if it affects women who are immunosuppressed or with particular pathologies (e.g. diabetes), vaginal candida can degenerate into a systemic condition, known as invasive candidiasis (or invasive candida ).
Invasive candida is the infection resulting from the passage of the fungus Candida albicans ( fungemia or funghemia ) into the blood and its spread to important organs, such as the heart ( endocarditis ), the brain ( encephalitis ), the eyes ( endophthalmitis ) or the bones ( osteomyelitis).
Invasive candida can be fatal for the patient, therefore it represents a medical emergency, to which immediate assistance must be given.
WHO IS MORE AT RISK OF INVASIVE CANDIDATE
Among women with vaginal candida, they are most at risk of invasive candidiasis:
- AIDS sufferers. As the reader will remember, AIDS affects the efficiency of the immune system;
- Those taking immunosuppressant drugs. This is the case, for example, of women undergoing an organ transplant;
- Those who are undergoing chemotherapy to treat a tumor. Chemotherapy has the side effect of reducing the efficiency of the immune system;
- People with diabetes mellitus. Diabetes promotes the proliferation of Candida albicans ;
- The subjects who must periodically resort to dialysis (the so-called dialysis). This is the case for women with renal insufficiency ;
- Those who, thanks to a certain health condition, must undergo the insertion of a central venous catheter . The central venous catheter is a medical device used in long-term therapies, to administer liquids, drugs and other substances that the human body needs in the presence of certain conditions.
Consequences of Vaginal Candidiasis in Pregnancy
In the absence of adequate care, vaginal candida in pregnant women represents a risk factor for premature birth (or preterm birth ).
Furthermore, in a very small percentage of pregnant women with vaginal candida, the infection can be transmitted to the baby at the time of delivery, resulting in a condition known as the newborn’s (or neonatal candida ) congenital candida .
When and to whom should I contact?
The appearance of suspicious symptoms, such as pain and itching at the genital level and pain during urination and during sexual intercourse, should prompt you to contact your general practitioner immediately, who will most likely prescribe a specialist visit to a gynecologist .
Main situations in which, in case of vaginal candida, it is good to contact the doctor:
- When it is the first time that you suffer from vaginal candida;
- When the patient is under 16 or over 60;
- When the patient is pregnant or breastfeeding;
- When the symptoms include leaks of foul smelling liquid and / or leaks of blood;
- When the patient has experienced at least two episodes of vaginal candida in the past 6 months.
Vaginal Candidiasis Diagnosis
Generally, for the diagnosis of vaginal candida, an accurate physical examination is sufficient , during which the doctor analyzes the symptomatic picture in detail, and a careful evaluation of the patient’s clinical history (or anamnesis ).
In special situations, however, it may happen that it is necessary to resort also to the execution of laboratory tests , such as the ‘ analysis of blood , l’ examination of urine and vaginal swab .
When are laboratory tests needed?
- When doubts persist about the nature of the present infection;
- When the symptoms of vaginal candida are severe or persist despite treatment;
- When vaginal candida is, for no clear reason, a recurrent condition.
How to behave in case of recurrent Vaginal Candida
Generally, women who repeatedly suffer from vaginal candida are people at risk (e.g. diabetes sufferers), aware of the reason behind the recurrence of the infection.
When this is not the case, however, they should undergo diagnostic tests to find out why repeated episodes of vaginal candida; the diagnostic tests indicated include: blood test, urine test and vaginal swab.
How to behave when you fall ill with Candida Vaginale for the first time
Women who develop vaginal candida for the first time must undergo a thorough medical examination, which includes, in addition to observing the symptoms, also the evaluation of the clinical history.
The information that emerges from clinical history is of fundamental importance for understanding the precise factors triggering vaginal candidiasis and for planning the most appropriate therapeutic plan.
If the doctor has doubts or believes it is possible to have a serious, undiagnosed, favorable disease (such as diabetes), he will most likely resort to the diagnostic tests already mentioned several times, i.e. the blood test, the examination of the urine and vaginal swab.
Vaginal Candidiasis Therapy
How is Candida Vaginale treated?
The treatment of vaginal candida is based primarily on the use of antifungal drugs , ie medicines with specific anti-fungal power; secondly, it provides particular attention to personal hygiene and temporary abstention from sexual activity .
Antifungal drugs for Vaginal Candida
Currently, on the market, antifungal drugs that can be used in the presence of vaginal candida are present in three formulations:
- In cream ( topical antifungals );
- In tablet for vaginal use ( antifungals for vaginal use );
- In tablet for oral use ( oral antifungals ).
TOPICAL ANTIMICOTICS
Topical antifungals for the treatment of vaginal candida are drugs in the form of a cream to be spread on the genital areas affected by the infection (vulva and vagina).
Topical antifungals used in the presence of vaginal candida include clotrimazole , econazole , fenticonazole nitrate , miconazole and nystatin .
With the exception of nystatin (which is an antibiotic with antifungal action), clotrimazole, econazole, fenticonazole nitrate and miconazole belong to the category of so-called imidazole derivatives (or imidazole derivatives ); imidazole derivatives are antifungal drugs which exert their power by destroying the cell membrane of fungi.
VAGINAL ANTIMICOTICS FOR USE
Vaginal antifungals for the treatment of vaginal candida are drugs in tablet form to be inserted into the vagina.Among the vaginal antifungals used in the presence of vaginal candida are the aforementioned clotrimazole, econazole, fenticonazole nitrate, miconazole and nystatin (they are the tablet version for vaginal use of the cream ones previously mentioned).
Possible side effects of clotrimazole, econazole and fenticonazole nitrate (both topically and vaginally): local burning and skin irritation.
ORAL ANTIMICOTICS
Oral antifungals for the treatment of vaginal candida are drugs in tablet form to be swallowed by mouth.
Among the oral antifungals used in the presence of vaginal candida, fluconazole and itraconazole stand out .
Fluconazole and itraconazole belong to the category of triazoles ; characterized by an anti-fungal power stronger than imidazole derivatives, triazoles act against certain enzymes that fungi like Candida albicans use to reproduce and survive (in simpler words, they destroy essential molecules for the reproduction of fungi).
Possible side effects of fluconazole and itraconazole: nausea , abdominal pain , diarrhea and flatulence .
Attention to Personal Hygiene
Paying attention to personal hygiene is a fundamental part of the treatment of vaginal candida.
In this sense, the rules to follow include:
- Use of good quality intimate cleaners , so as not to irritate the already suffering genital area;
- Be careful, after each shower, to dry the genital areas .
Did you know that …
In case of vaginal candida, in order to keep the private parts as dry as possible, doctors recommend the use of wide and not compressing underpants .
Temporary abstention from sexual activity
Although the use of condoms prevents the transmission of vaginal candida, doctors advise avoiding sexual intercourse with your partner for the duration of the treatment and to resume only after healing has taken place.
It should be noted that the condom and the contraceptive diaphragm are sensitive to topical antifungals and vaginal use antimitotics, where sensitive means that they could be damaged; any damage to these methods of contraception could be not only the cause of the transmission of vaginal candida, but also of an unwanted pregnancy.
Treatment of Vaginal Candidiasis in Pregnancy
Before taking any medication, pregnant women who develop vaginal candida should consult their doctor and gynecologist in order to find out which drug is most suitable for them.
In general, antifungal therapy based on clotrimazole or nystatin in the form of tablets for vaginal use is provided for pregnant women suffering from vaginal candida.
Prevention
The main measures to prevent vaginal candida are:
- Do not abuse antibiotics (follow the administration procedures indicated by the attending physician);
- In the presence of conditions conducive to candida (eg: diabetes, AIDS, immunosuppression from chemotherapy, pregnancy, etc.), take maximum care of personal hygiene and avoid sexual intercourse with people infected with Candida albicans ;
- Wash the private parts with quality detergents;
- Thoroughly dry your private parts after each shower.
Vaginal Candidiasis Prognosis
If it is not a recurrent condition and the patient generally enjoys good health, vaginal candida tends to have a benign prognosis.
Vaginal Candida Healing Times?
If treatment is timely and adequate, vaginal candida usually heals within 7-14 days .
If vaginal candida persists beyond the time indicated above, a doctor should be consulted immediately.
Vaginal candidiasis, also known as a yeast infection, is a common condition. Here’s a tabular format summarizing its symptoms and treatments:
| Aspect | Details |
|---|---|
| Symptoms | – Itching and irritation in the vagina and vulva |
| – A burning sensation, especially during intercourse or while urinating | |
| – Redness and swelling of the vulva | |
| – Vaginal pain and soreness | |
| – Vaginal rash | |
| – Thick, white, odor-free vaginal discharge with a cottage cheese appearance | |
| – Watery vaginal discharge | |
| Treatments | – Antifungal creams, ointments, tablets, and suppositories (e.g., clotrimazole, miconazole) |
| – Oral antifungal medication (e.g., fluconazole) | |
| – Maintaining good genital hygiene | |
| – Avoiding scented hygiene products and douches | |
| – Wearing loose, breathable cotton underwear | |
| – Avoiding hot baths and hot tubs | |
| – Eating yogurt with live cultures or taking probiotics |
It’s important to consult a healthcare provider for an accurate diagnosis and appropriate treatment, as symptoms of vaginal candidiasis can be similar to other conditions.
