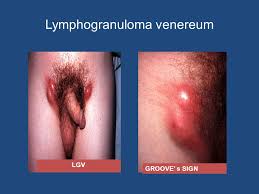
Lymphogranuloma venereum (lvg) is a systemic infectious disease caused by a filter- passing agent and transmitted by sexual contact. The disease is characterized by the appearance of a small genital ulceration followed by suppuration of the regional lymph nodes, mild constitutional symptoms, and, occasionally, inflammatory lesions in various tissues of the. body. Late manifestations of the disease consist of chronic ulcerative lesions and fibrotic changes in the genital tract and rectum.
Lymphogranuloma Venereum Etiology.
The agent causing lymphogranuloma venereum is a member of the psittacosis- lymphogranuloma group of filter-passing agents. These agents have common morphologic and immunologic characteristics that include large particle size, susceptibility to antimicrobial drugs, and cross reactivity in serological tests. Strictly speaking, these filter-passing agents are not true viruses, but for convenience the terms virus and agent are used interchangeably here (see Psittacosis, Trachoma). The virus of lymphogranuloma produces meningoencephalitis in mice following intracerebral inoculation. It can be cultured in the yolk sac of the chick embryo, in which viral particles subjected to special staining methods can be seen with an ordinary microscope. Antigens. prepared from the infected yolk material have been used for intradermal diagnostic (Frei) tests and for complement-fixation tests.
Prevalence and Incidence.
Lymphogranuloma venereum is widely distributed throughout the world, but it is probably most prevalent in the tropics. Once a frequent cause of venereal disease among Negroes in the southern United States, the disease now appears less frequently. Surveys based on serologic methods during World War II showed a prevalence as high as one third of the adult southern Negro population, but in 1966 only 625 new cases were reported in all of the country. There is evidence to indicate that the incidence of the disease in the United States may increase because of spread of the infection by American soldiers returning from Southeast Asia. The illness has been described throughout the world under various names, such as tropical bubo climatic bubo, lymphogranuloma inguinale, and lymphopathia venereum.
Pathogenesis of Lymphogranuloma venereum.
Approximately three to thirty days after sexual exposure, a small transient ulceration usually appears at the site of inoculation. This is followed within a few days by enlargement and suppuration of the regional lymph nodes, the so-called bubo. The virus is disseminated at this time throughout the body, and has been recovered from the blood and cerebrospinal fluid as well as from the lymph nodes draining the primary lesion. Systemic lesions consisting of arthritis, cutaneous lesions, and ocular manifestations (iritis and keratitis may develop in the early stages of the illness. These initial symptoms may disappear spontaneously, and the patient may become asymptomatic for many years. A small but undetermined percentage of patients later develop chronic ulcerative lesions about the rectum and genitalia.Shortly after the onset of lymphadenitis, complement-fixing humoral antibodies, skin reactivity to the viral antigen, and elevation of the serum globulin develop. These immune reactions may persist for many years.
Clinical Manifestations.
The primary lesion of lymphogranuloma consists of a shallow, painless ulceration a few millimeters in diameter. It is often inconspicuous, and may pass unnoticed by the patient. In such cases the regional lymphadenitis may be the first evidence of the disease. Occasionally a pea-sized nodule, called a bubon- ulus, may develop in the lymphatics draining the primary lesion.
The painful enlargement and inflammation of the lymph nodes in one or both inguinal areas are the most conspicuous early features of the disease. The lymph nodes often become matted together to form conglomerate tender masses above and below the inguinal ligament. Within a few days suppuration develops and the overlying skin may ulcerate, with the formation of multiple chronic draining sinuses. The lymphadenitis is often accompanied by systemic manifestations of malaise, myalgia, and fever, and occasionally by arthritis or conjunctivitis. In rare instances, meningitis and pericarditis have been observed.
In untreated cases, suppuration and drainage of the lymph nodes may persist for several weeks or months, but eventually spontaneous healing takes place. After a few years, however, chronic ulcerative lesions and fibrotic changes may develop on the external genitalia. In women, dense fibrous strictures of the rectum and purulent proctitis are not uncommon and may be associated with destructive lesions in the vaginal tissues.
Another late manifestation is elephantiasis of the external genitalia, which is caused by obstruction of lymphatic channels. Proctitis and its sequelae may also be observed in homosexual men. These late complications are sometimes associated with a profound anemia, loss of weight, and severe cachexia. In a few instances death results.
Diagnosis of VIG.
The diagnosis of lymphogranuloma is usually made on the basis of its clinical manifestations, but the demonstration of specific skin reactivity and complement-fixing antibodies may be needed to confirm the diagnosis.
Differentiation fiom chancroid infection may be difficult, as the genital ulceration and regional lymph node involvement in both diseases may be similar. The etiologic agent of chancroid, the Ducrey bacillus, is often found in stained smears or cultures of the purulent exudate in the undermined edges of the genital lesion. The inguinal nodes in both illnesses may enlarge to form a painful suppurative mass which, in chancroid infection, may rupture to form a single large ulceration, whereas, in lymphogranuloma venereum, the lymph nodes have multilocular areas of fluctuation that rupture to form multiple draining fistulas.
Lymphogranuloma must also be differentiated from other conditions producing lymphadenopathy in the inguinal area such as syphilis, pyogenic infections, and neoplasms. Isolation of the virus is not practicable except perhaps in selected cases of meningitis, arthritis, or iritis. In such patients, an attempt should be made to obtain the virus from the involved tissues or from enlarged lymph nodes. A positive reaction to the commercial skin test antigen (Lygranum) will appear in a week or two in practically every patient with the disease. The skin test ‘to this antigen as well as that made from the Ducrey bacillus must be interpreted with caution, because positive reactions may persist for many years after a previous infection. A two- or threefold change in titer of complement-fixing antibodies, however, is usually considered diagnostic of an active infection.
Hyperglobulinemia is a common finding, and may at times be helpful in the diagnosis. The diagnosis can also be made by biopsy of the primary lesion or enlarged lymph nodes. The histologic appearance of lymphogranuloma venereum consists of a rather characteristic granuloma with abscess formation that can usually be differentiated from chancroid and other infections.
Treatment of Lymphogranuloma Venereum
Surgical treatment is usually necessary for the late manifestations of the disease such as rectal stricture and elephantiasis. No attempt should be made, however, to excise the inguinal buboes, but repeated aspirations of the suppurating lymph nodes may be necessary to prevent the formation of chronic draining sinuses.
Prevention of LVG
There is no specific vaccine against lymphogranuloma venereum. There is some reason to believe that careful washing of the bacterial superinfection. Rug therapy has no influence on established scars or pannus. Surgical correction is required in serious entropion or trichiasis. Topical corticosteroids and caustics have no place in therapy. Prevention. Endemic trachoma is favored by ignorance, poverty, and cultural patterns that oppose hygienic improvement and medical treatment. In addition, the sheer lack of water available for washing seems to be important.
The most potent preventive measures include efforts to increase the total supply of water, simple cleanliness such as frequent hand washing, avoidance of common towel or common eye pencil, and measures to reduce flies. It is also important to detect mild, early infection in young children in areas and to apply effective drug treatment repeatedly. This prevents the blinding progression, and probably reduces the infective reservoir. Detection and treatment of adults who already suffer visual impairment can probably the source of infection for children.
Prevention of genital TEX infections requires the .control of sexual promiscuity, early diagnosis and effective treatment :: cases and sexual contacts, and prolonged establish that the genital or ocular infection is not relapsing. Effective treatment or pregnant women with genital TRIC infection can prevent inclusion conjunctivitis in the newborn The usual instillations into the eye of the newborn silver nitrate or penicillin) do not prevent inclusion conjunctivitis. A newborn baby with inclusion conjunctivitis should be isolated to prevent spread to others.
Experimental vaccines against TRIC infections have been prepared. In field tests no vaccine has given unequivocal protection against infection, or against progression of disease Work is continuing in the hope of developing preparations of greater immunogenicity. However, natural infection engenders only minimal protection against reinfection. The most that could be expected of artificial immunization is an attenuation of the disease resulting from infection. The best current hope for control of TRIC infections rests on a combination of public health measures and drug treatment.
Lymphogranuloma venereum (LGV) is a sexually transmitted infection caused by certain types of the bacterium Chlamydia trachomatis. The treatment for LGV is typically antibiotic therapy. Here is a guide in a tabular format outlining the recommended treatment for LGV:
| Stage of Infection | Treatment | Duration | Notes |
|---|---|---|---|
| Primary LGV (small, painless sore on the genitalia) | Doxycycline 100 mg orally twice a day | 21 days | Alternative: Erythromycin 500 mg orally four times a day |
| Secondary LGV (swollen lymph nodes, flu-like symptoms) | Doxycycline 100 mg orally twice a day | 21 days | If doxycycline is contraindicated, consider Erythromycin or Azithromycin |
| Tertiary LGV (chronic, progressive lymph node enlargement) | Doxycycline 100 mg orally twice a day | Minimum 21 days, extend based on clinical response | Surgery may be required for draining abscesses |
Additional Notes:
- Pregnant women: Azithromycin is preferred due to contraindications for doxycycline in pregnancy.
- Allergic to Tetracycline: Erythromycin or Azithromycin can be used as alternatives.
- Monitoring and Follow-up: Patients should be followed up until signs and symptoms have completely resolved.
- Sexual Partners: Sexual partners should be examined and treated if they had sexual contact with the patient within the 60 days before onset of symptoms.
Prevention Tips:
- Practice safe sex, including the use of condoms.
- Regular screening for sexually transmitted infections if at risk.
- Avoid sexual contact while being treated for LGV.
It’s important to consult a healthcare provider for a definitive diagnosis and treatment plan, as this information is meant for general guidance only.