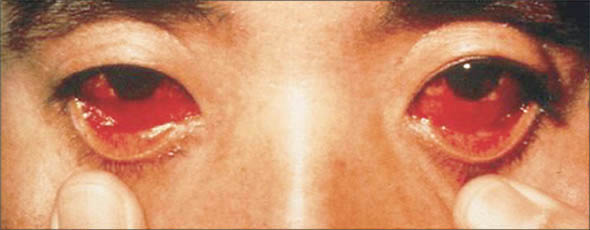
Epidemic hemorrhagic fever is an acute disease of unknown cause that occurs during the spring and autumn in northeastern Asia It is characterized by fever, prostrationr, prostration, omiting, proteinuria, hemorrhagic manifestations, shock, and renal failure.
History.
This disease was first described in the far east of the Soviet Union in the 1930’s. The Soviets call the disease hemorrhagic nephroso-nephritis or hemorrhagic fever with renal syndrome, and 300 to 500 cases are still recorded annually from that region. Western physicians first encountered it in 1951 in the form of a seasonal epidemic occurring among UN troops in Korea. It was then learned that the Japanese had observed an identical clinical disease in eastern Manchuria, which they designated epidemic hemorrhagic fever.
Etiology.
Soviet investigators reproduced the disease in human volunteers by the parenteral injection of serum or urine obtained prior to the fifth day of illness from patients with the naturally occurring disease. They further found that the disease agent was filterable through a Berkefeld filter’ (grade N), that the incubation period was usually 12 to 16 days, and that a single attack conferred immunity. After years of failure, Soviet virologists claim (1969) to have isolated the causative agent in human and porcine kidney cell cultures, using fluorescent antibody technique as marker of viral replication. Acute and convalescent human sera showed specific antibody increases to this agent, which is not yet available outside the Soviet Union for confirmatory study.
Epidemiology of Epidemic Hemorrhagic Fever.
The endemic area includes far eastern Siberia, parts of eastern Manchuria, and Korea north of Seoul. Sporadic cases occur throughout the year, but the large majority are recorded during late spring and autumn. All ages and races and both sexes are susceptible, but adult males usually experience the highest number of attacks. The disease is rural, and is. characterized by isolated cases widely separated in place. Environmental exposure to forests or fields near forests is invariably noted. Person-to-person transmission does not occur.
Since World War II Soviet scientists have studied many outbreaks in forested regions west of the Ural Mountains of what they now believe to be an identical disease. Other reports of similar disease have been made from northern Scandinavia, Czechoslovakia, Rumania, and Bulgaria. Although the incidence and severity of hemorrhagic manifestations and mortality are lower than in northeast Asia, the renal lesion is apparently the same. The epidemiology is also similar, with one important difference.
The largest epidemics were marked by a slowly accumulating number of cases beginning in late spring, culminating in an often explosive burst between November and January. In these remarkable outbreaks the peak of the epidemic was preceded by an eruption of cyclically large forest rodent populations (usually the red-backed vole Clethriono-mys glareolus) into the fields, barns, and even houses of people living in or next to forests. These rodent “invasions” were probably precipitated by meteorologic conditions unfavorable for winter survival of the animal s (rain and sleet instead of a snow blanket). Only under these conditions were multiple cases in the same family frequently observed. On the basis of these data Soviet workers now believe that epidemic hemorrhagic fever is transmitted directly from asymptomatically infected rodents to man by means of virus-contaminated rodent excreta.
Pathology.
Profound, protein-rich retroperitoneal edema is characteristic of early death in shock, but not of later deaths. Changes in various organs apparently have a similar pathogenesis and consist of widespread, often focal, congestion and hemorrhage, sometimes accompanied by necrosis, without significant inflammatory response. The “pathognomonic” lesion is found in the kidneys, which appear swollen, and when incised exhibit extreme hemorrhagic congestion sharply localized to the medulla. Gross congestion or hemorrhage derived from dilated, congested small blood vessels is also found frequently in the right atrium, the pituitary, and the stomach; less often in intestines, adrenals, lungs, and central nervous system. Liver and spleen are usually not grossly involved. Petechial hemorrhages may occur in the skin, heart, adrenals, brain, and serous surfaces.
Clinical Course and Pathologic Physiology.
The clinical and laboratory manifestations of hemorrhagic fever make up a confusing array of problems that occur in rapid sequence with considerable overlapping and variation in severity. However, many patients follow a fairly typical course that is conveniently considered in relation to several phases. Although all patients exhibit proteinuria and many have petechiae and some degree of hemoconcentration, the hypotension and renal failure, and such consequences as shock, serious hemorrhages, and fluid and electrolyte imbalances, occur in no more than 20 per cent.
The febrile phase lasts three to eight days and i_s characterized by fever, malaise, a flush of the face and neck, injection of the eyes and palate, and other nonspecific features. Evidence of widespread vascular dysfunction appears at this time. Toward the end of the febrile phase, petechiae occur, blood platelets decrease, the hematocrit begins to increase, and faint traces of protein appear in the urine.
The hypotensive phase develops suddenly during defervescence and generally lasts one to three days. Despite shock, which accounts for a third of all deaths, the extremities may remain warm, and arteriolar dysfunction may contribute to the hypotension. The dominant feature, however, is a reduction in blood volume owing to loss of plasma from the vascular system, as evidenced by a rapid increase in hematocrit to as high as 70 per cent and to trapping of erythrocytes in dilated capillaries. Heavy proteinuria, oliguria, acute renal failure, and hemorrhages of capillary origin associated with thrombocytopenia are prominent clinical features, whether or not hypotension develops. Nausea and vomiting are common. Backache and particularly abdominal pain resulting from localized edema have occasioned exploratory laparotomy in certain misdiagnosed instances. The leukocytes, which earlier Vwere normal or reduced, now show a leukemoid reaction.
The oliguric phase begins as the hematocrit decreases and the sequestered plasma returns to the vascular system. It usually lasts for three to five days. Deaths in this phase are due to pulmonary edema, electrolyte abnormalities, and shock secondary to dehydration or pulmonary infections. This phase is one of increasing renal failure and nitrogen retention, continued vomiting, and dehydration. Hyperkalemia is common. Despite improvement in many of the earlier symptoms, increasing confusion and extreme restlessness are common, as is hypertension. Some patients exhibit a hypervolemic syndrome that may respond to phlebotomy. Hemorrhages into the skin, sclerae, gastrointestinal tract, lungs, and renal pelvis continue, but rarely are large in amount and generally decrease toward the end of the oliguric phase.
The diuretic phase, which may last for days or weeks, usually initiates clinical recovery and rapid improvement in renal function. However, a diuresis of 3 to 8 liters daily represents a hazard to patients who are already extremely dehydrated and who have had limited caloric intake for seven to ten days. These patients exhibit a brittle fluid volume homeostasis and may fluctuate rapidly between shock, on the one hand, and hypertension and pulmonary edema, on the other, depending on the state of the fluid balance. Serious potassium deficiency may occur, and hypernatremia can be troublesome. Deaths in this phase account for a third of the total, and are usually due to shock secondary to dehydration and to pulmonary complications, including bacterial infections. The diuresis characteristic of this phase does not represent mobilization of edema fluid, but is the result of residual renal tubular damage.
Convalescence requires three to twelve weeks and is characterized by gradual return to normal of appetite, strength, and urinary concentrating ability.
Epidemic Hemorrhagic Fever Diagnosis.
In the absence of any specific test, the diagnosis must be made on clinical evidence and should be suspected when an acute febrile illness Associated with the characteristic flush and petechiae occurs in a subject who has been in an endemic area. The subsequent developments such as hypotension or shock, increased hematocrit, thrombocytopenia, oliguria, and renal failure assist in establishing the diagnosis, but proteinuria and isohyposthenuria developing near the time, of defervescence are the most useful diagnostic signs.
Prognosis.
The case fatality rate, once techniques for prompt diagnosis and early, adequate treatment were developed, has been 5 per cent or less. No single finding is of great prognostic value in individual patients. However, prolonged high fever, protracted or recurrent shock, and persistent hemoconcentration are all ominous features. With rare exceptions, survivors who have not had central nervous system hemorrhages make apparently complete recoveries.
Epidemic Hemorrhagic Fever Treatment.
Because antimicrobial drugs, convalescent serum, hormones, and other agents are entirely ineffective, the management of hemorrhagic fever must be supportive and based on an understanding of its physiologic and biochemical characteristics and on frequent clinical observations. Adequate sedation with barbiturates or opiates is frequently required for restlessness. Contrary to the practice in other febrile diseases, fluid intake must be limited because any excess will simply leak out of damaged capillaries and increase edema and symptoms.
When intravenous fluid is required, it usually should be 10 per cent dextrose in water, and must be given very slowly. If shock fails to respond to simple measures such as shock blocks, then concentrated (salt-poor) human serum albumin to restore plasma volume and continuous intravenous infusion of pressor drugs such as norepinephrine may be required. Doses of the latter must be based on the response of the shock, blood pressure, and hematocrit. Occasionally, large doses of both albumin and pressor drugs are required.
Treatment in the oliguric phase is that of acute renal failure, with careful control of electrolytes and particular attention to hyperkalemia. If oliguria persists, hemodialysis or peritoneal dialysis is indicated. Soviet workers have treated 60 severe cases -with an “artificial kidney” and report only three deaths. Phlebotomy may be required for the fully developed hypervolemic syndrome. The chief problem of the diuretic phase is one of careful matching of fluid and electrolyte intake against the brisk, urinary output, so as to avoid excessive dehydration and shock, on the one hand, and hypervolemia and pulmonary edema, on the other. Electrolyte abnormalities are still a problem, especially potassium deficiency.
Prevention of Epidemic Hemorrhagic Fever.
Preventive measures are based on the assumption that the disease is transmitted by rodents with or without the aid of an associated arthropod parasite. Vigorous rodent control measures, as well as dipping of clothing in acaracidal solutions and the individual use of insect repellents, are recommended in endemic areas during seasons} periods ol disease activity.
Conclusion
In conclusion, Epidemic Hemorrhagic Fever is a severe and potentially fatal illness caused by various viruses. Understanding the causes, symptoms, and prevention strategies associated with this disease is essential for both healthcare professionals and the general public. By taking appropriate precautions and following proper hygiene practices, we can collectively work towards minimizing the impact of Epidemic Hemorrhagic Fever and safeguarding public health.