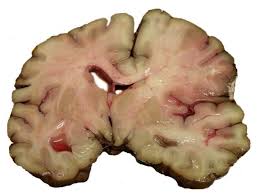
Cerebral infarction resulting from cerebral emboli or from cerebral atherosclerosis and thrombosis, respectively, cannot be distinguished by the neurologic disorders they produce. Differences between these two causes of infarction do exist, however, in the mode of onset of symptoms and in the general physical evaluation.
Causes And Symptoms of Cerebral Infarction
The pattern of onset of neurologic symptoms and signs in cerebral infarction often suggests the cause. Cerebral embolism causes an abrupt onset of symptoms, and headache often precedes other neurologic symptoms by several hours. Cerebral infarction due to atherosclerotic vascular obstruction or occlusion often has a less sudden onset. There may be a distinct series of steplike increases in neurologic symptoms and signs, or infarction may be preceded by a series of transient ischemic attacks.
A gradual onset with increasing neurologic deficit over several (one to five) hours is characteristic of the progressing stroke. A gradual onset of. symptoms and signs over two days or, occasionally, one week, does occur but is uncommon. The frequency of these different patterns can be inferred from the experience of one large series of patients with ischemic infarction; about one third had a sudden onset of symptoms, about one fifth had symptoms that progressively increased over one to 12 hours, and only about one in 20 had symptoms that progressed for as long as 12 to 24 hours. One fifth of the patients with occlusive vascular disease and cerebral embolism had the onset Of neurologic signs during sleep.
Headache is present in many patients with embolic or atherosclerotic infarction. The headache is usually mild and localized to the side of the infarction. Headache is believed to be caused by vasodilation of unoccluded vessels near the in- farcted area, and is most common when vessels near the base of the brain are occluded.
Consciousness is usually not lost at the onset of infarction of the cerebral hemispheres, but may be reduced, particularly when large infarcts strike the dominant hemisphere. When unconsciousness is present from the onset or is the initial symptom, brainstem infarction is the most likely cause. When large hemispheric infarctions are complicated by rapidly developing and severe brain edema, loss of consciousness due to diencephalic and upper brainstem compression may occur shortly after the onset of symptoms.
This may give the false impression of loss of consciousness from the onset unless a careful history documents a lucid period at the very beginning of symptoms. Convulsive seizures are rare at the onset of cerebral infarction, but they occur in about 8 per cent of patients sometime in the course of the acute or convalescent phase of the illness. They are usually focal, but may be generalized.
When infarction is limited to the cerebral hemisphere, there is weakness or paralysis in the extremities contralateral to the infarction. Patients may also be aware that sensory perception on the side of weakness is impaired and may complain of heaviness or numbness in the arm or leg. They rarely have other sensory symptoms such as pain or paresthesias. Defects in visual fields are common but often escape the patient’s notice. The defect is suspected when patients pay little attention to visual stimuli on one side of the body. At times, the eyes may be constantly deviated to the side away from the neurologic deficits.
The most serious consequence of infarction in the dominant hemisphere is dysphasia, which can range from a mild deficit of expression to aphonic mutism. The dysphasia is almost invariably a mixture of difficulty with expression (expressive dysphasia) and difficulty in understanding what is said, written, or indicated by gesture (receptive dysphasia); one or the other may predominate.
In patients who have infarction in the nondominant hemisphere, lack of awareness or concern about paralysis of the contralateral side is often evident. Such subjects may, at times, be so completely unaware of their neurologic disabilities that they are hospitalized only after family or friends notice their disabilities. This phenomenon, anosognosia, is most common when a patient is obtunded and when there is a significant sensory deficit on the paretic side as a result of infarction of the parietal lobe. It accompanies nearly one fourth of all large strokes, but usually persists only if the patient remains obtunded or confused or has little return of sensation.
Infarctions in the brainstem produce a wide variety of symptoms. Among the most conspicuous are vertigo, diplopia, dysarthria, dysphagia, and ataxia. In addition, the patient may note unilateral or bilateral sensory impairment or weakness. Often patients note clumsiness and difficulty in performing skilled acts without paresis.
A “Cerebral Infarction” refers to a type of stroke that occurs when the blood supply to a part of the brain is interrupted or reduced, depriving brain tissue of oxygen and nutrients. This can happen due to various reasons, including blood clots. The affected brain cells can begin to die within minutes.
Conclusion
Cerebral infarction is a serious condition that can have life-altering consequences. Understanding the causes, symptoms, and treatment options is crucial for early detection and effective management. By adopting a healthy lifestyle and managing risk factors, individuals can reduce their chances of experiencing a cerebral infarction. If you or someone you know exhibits symptoms of stroke, do not hesitate to seek immediate medical attention. Remember, time is of the essence when it comes to treating cerebral infarction.