Cat scratch disease is lymphatics, usually limited to one anatomic region, developing as a sequel to accidental injury of the skin. In two thirds of the reported cases there has been a history of scratch or bite by a cat.
Epidemiology.
The disease occurs in all parts of the world, most often in winter. Children are affected more frequently than adults. Although injuries by cat claws or teeth are the most common form of skin injury, other puncture wounds, by wood splinters, thorns, and metallic objects have appeared to be responsible at times. Cats thought to have caused human infection show no sign of illness, do not react to the cat-scratch antigen, and probably merely convey the causative agent on claws or teeth. “Epidemics” of cat scratch disease, though reported, are difficult to evaluate because they may simply reflect special interest and awareness of certain physicians. There are, however, several reports of more than one case developing in a family over a period of a few months.
Etiology.
Although this disease has the features of a specific infection, efforts to demonstrate a causative bacterium, fungus, or filterable virus have met with failure. Perhaps the most impressive evidence for viral etiology is in a report of electron microscopic examination of affected lymphatic tissue, in which herpes-like viral particles were observed. The hypothesis has been offered that the clinical manifestations result from an immunologic reaction; hence the inciting agent may no longer be demonstrable at the time the patient seeks medical help. Several groups of workers have reported serologic evidence that the causative agent is related to viruses of the psittaco-sis-ornithosis-lymphogranuloma venereum-tra-choma group, but the proportion of patients exhibiting such positive serologic reactions has varied considerably, and, fu with cat scratch disease do not react to intradermal injection of antigens prepared from this group of viruses.
Pathogenesis.
An indolent or subacute inflammatory lesion develops at the site of primary inoculation in approximately one third of cases. It becomes clinically evident one to several weeks after the injury. Lymphadenitis, the hallmark of the disease, appears a few days later. Initially this takes the form of a granulomatous inflammation, sometimes containing giant cells. In cases of some duration micro-abscesses can nearly always be found; in about one fourth of cases these coalesce to form a grossly evident abscess.
Clinical Manifestations.
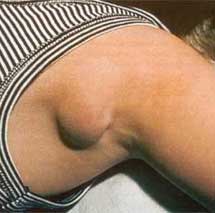
The site of inoculation is most likely to be on the hand, forearm, or face. It may exhibit one or more erythematous papules. Less frequently there is vesicle formation going on to rupture and production of a small eschar. The lesion usually heals without scar formation. The lymph nodes most frequently affected are in the epitrochlear, axillary, or cervical groups, but when the injury has been on the legs the inguinal nodes may be the site of the disease. The process varies in clinical severity and acuteness, sometimes smoldering for weeks with enlarged and tender nodes, at other times progressing more quickly to pronounced swelling, with redness and edema of the overlying skin.
There may be fluctuation, and in rare instances the skin undergoes necrosis,’ permitting discharge of exudate. The usual course is for the swelling and’ tenderness gradually to subside in two to eight weeks. Systemic manifestations are not prominent, although young children sometimes have high fever for a few days. The erythrocyte sedimentation rate may be elevated; there is often a moderate leukocytosis, and sometimes mild eosinophilia. Transient morbilliform rashes may accompany the adenitis; occasionally lesions are developed which have the appearance of erythema nodosum. Pulmonary and arthritic manifestations are extremely rare, perhaps only coincidental. Development of osteolytic lesions near the adenitis Yvas been described.
The most serious complication is encephalitis, evidenced by fever, delirium, cranial’nerve palsies, and pleocytosis in the cerebrospinal fluid. The encephalitis usually subsides without residual damage. When the primary lesion affects the conjunctiva, the preauricular nodes are affected, giving the clinical picture of Parinaud’s oculo-glandular syndrome.
It has been suggested that cat scratch disease may present as mesenteric lymphadenitis, because positive skin tests have been associated with that clinical picture. The presumption is that the portal of entry in such cases is the intestine.
Cat Scratch Disease Diagnosis.
The diagnosis is based largely on the clinical circumstances, i.e., a subacute lymphadenitis limited to one region with or without suppuration, with or without a primary skin lesion distal to the node, and history of cat scratch or bite or of some comparable trauma to the skin. Several other processes must be considered in the JJ/fereatiaidiagnosis. Among infections are tuberculosis, infectious mononucleosis, tularemia, lymphogranuloma venereum, and sporotrichosis. Hodgkin’s disease may cause difficulty, because the granulomatous picture in the lymph node of cat scratch disease may bear some resemblance to that of Hodgkin’s disease; but the presence of micro-abscesses usually serves to differentiate these.
The Hanger-Rose test appears to be relatively specific for cat scratch disease. This employs an “antigen” prepared from the purulent matter aspirated from nodes of other patients, in a manner comparable with that formerly employed for lymphogranuloma venereum (Frei test). The exudate is diluted 1 to 5 in saline, and sterilized by heating at 6 7 C f or cne hour on two occasions. After intraderrr.il injection of this material, the reaction is read at 24 to 48 hours. A positive result consists of induration 5 mm. or more and erythema 10 mm. or more in diameter. Unfortunately test material is not available commercially.
Cat Scratch Disease Treatment.
There is no evidence that antimicrobial therapy, including tetracycline, is of value. Bed rest is advisable when fever and general malaise are present. If fluctuation becomes evident in the affected lymph node, it is recommended that the pus be aspirated (and used for the preparation of skin test antigen). Incision of an abscess is inadvisable, because sinus formation with prolonged drainage sometimes results, but biopsy of intact nodes seems safe in the pre-suppurative stage