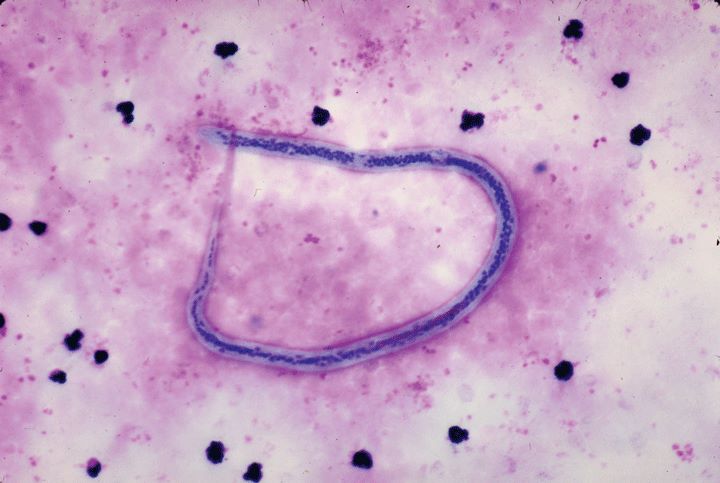
Wuchereria bancrofti is a Filariasis that inhabits the tropical and subtropical areas . The disease usually is not fatal, but can cause abscesses and severe damage leading to disability. The adult worms reside in the lymphatic system and produce recurrent lymphangitis with fibrosis and obstruction. The infection is transmitted by culicine and anopheline mosquitoes.
The threadlike adult worms are 4 to 10 cm. long and live for decades. The female worm is viviparous, producing microfilariae 130 to 320 fx long which are found in the peripheral blood; in some forms this occurs only at night, whereas during the day the microfilariae are in the lungs. If ingested by a suitable mosquito, these microfilariae develop in the thoracic muscles of the insect and are present in the mouth parts after two weeks. They enter the skin through the puncture wound when the mosquito next feeds, and finding their way to the lymphatics of the host the males and females mate and mature. More than a year after infection microfilariae appear in the peripheral blood.
Epidemiology of Wuchereria Bancrofti .
Man is the only definitive host of this common type of filariasis. Periodic bancroftian filariasis is found throughout tropical Africa and North Africa, as well as in the tropical coastal borders of Asia and Queensland. It is endemic in the West Indies and the northern countries of South America. In the northern Pacific bancroftian filariasis exhibits nocturnal periodicity, but in the Pacific Islands east of 160 degrees of longitude (including New Caledonia, Fiji, Samoa, The Ellis and Cook islands, Society Islands, and the Marquesas) the microfilariae are nonperiodic, being present in the peripheral blood throughout the 24-hour period. The term W. bancrofti uar. pocifica has been applied to this strain.
Pathology of Wuchereria bancrofti .
The severity of the lesions probably depends on the adult worm load and their site of development and the susceptibility of the host Light infections are often asymptomatic, and microfilariae are detected on incidental blood examinations. Maturing adults in .the lymphatics are associated with endothelial thickening, fibrin deposition, and infiltration with eosinophils, histiocytes, and lymphocytes. Giant cells occur. Fibrotic and inflammatory changes tend to obstruct the lymphatics, and this process is exacerbated by death of the worms, which may calcify. There is reactive hyperplasia in the lymph nodes, and small granulomas are seen. An eosinophilic endophlebitis of the small veins, is present in the lymph nodes.
The testicles and epididymis often show similar changes with evidence of ‘chronic inflammation. Worms may not be present at the site of inflammation. Secretions of the worm, especially after molting, are thought to be responsible for some of these changes. As lymphatic obstruction becomes more extensive, chronic edema develops in the infected areas. Recently lymphedema has been produced in laboratory animals with longstanding bancrofti infections.
Clinical Manifestations of Wuchereria bancrofti Which Every Doctor Must Know.
Attacks of fever, headache, and lymphadenopathy sometimes associated with urticarial rashes are known as filarial fever and occur in the acute phase of the disease. Often, however, no history of this early phase can’ be obtained. Epididymitis may occur as a lone lesion. Lymphatics most affected are those of the inguinal region, upper arms, and spermatic cord. Chronic lymphadenopathy is often the only sign of infection for years. Retrograde lymphangitis may be noted.
In a small proportion of infected individuals, with increasing lymphatic obstruction over the years, all degrees of chronic edema occur, affecting especially the lower limbs and scrotum. Initially the edema is pitting, but as organization of collagen occurs in the edematous subcutaneous tissues, it becomes nonpitting. Eventually the giant limbs of elephantiasis are produced. The skin over the affected part, at first smooth, later becomes scaly and is fissured at the points where the fascia is attached to the skin. Hyperkeratosis produces warts and nodules. Varicose nodes in the groin are the result of lymphatic dilatation and may lead to scrotal lymphedema. Infection may supervene in any of these lesions with formation of a chronic discharging sinus. Chronic inflammatory disease of the testicle and epididymis with or without hydrocele occurs.
Chyluria may be renal or vesical in origin, depending on the level at which the lymph varix communicates with the urinary tract. Cystoscopy and intravenous or retrograde pyelography help to establish the site of communication.
Diagnosis of Wuchereria bancrofti .
In the early stages and when lym-phadenopathy only is present, microfilariae are usually present in night blood films. Although the motile microfilariae are easily seen in fresh films, staining is necessary for identification. Microfilariae may be absent in the late stage; thus, only 4 per cent of patients with elephantiasis and 30 per cent of patients with hydrocele had microfilariae in one series. Concentration techniques are available for microfilariae, and they may be found in the chylous urine or hydrocele fluid.
Eosinophilia is not a constant finding. The filarial complement-fixation test and skin test, although only group specific, are useful in suggesting a filarial cause for a lymphedema. Lymphangio-grams reveal the extent of the lymphatic obstruction and may be a useful preoperafive measure. It is rarely justified to remove an enlarged lymph node to find the adults because this still further prejudices the lymphatic circulation. In an endemic area surgeons frequently encounter adult worms when operating on the groin.
The differential diagnosis depends on the type of clinical syndrome. Lymphadenopathy caused by other infections and neoplasms must be considered. Elephantiasis may be associated with congenital defects of the lymphatic drainage as well as tuberculous inguinal lymphadenitis. Tuberculosis, Schistosoma haematobium, and gonorrhea produce epididymitis, and relatively few hydroceles are filarial. Lymphatic obstruction caused by many other agents may produce lymphedema and chyluria.
Treatment of Wuchereria bancrofti .
Diethylcarbamazine (Banocide, Het-razan) is believed to kill a large proportion of adults as well as microfilariae. A dose of 3 mg. per kilogram of body weight is given, rising to a maximum of 12 mg. per kilogram over four days. This dose is then given daily for 14 days. Reactions are mild in comparison with those seen in onchocerciasis, but fever, nausea and vomiting, and -kin rashes may occur as with any drug. The arsenical Mel W and the antimonial Astiban (sodium c:mer-captosuccinate) kill adult filariae, but are too toxic for general use. All patients with microfilaremia should receive an adequate course of treatment.
The management of lymphedema depends on its severity. Mild degrees are best treated with elevation of the foot of the bed and an elastic stocking. Careful instructions regarding foot care should be given, as ascending streptococcal cellulitis is common in the edematous tissues and further prejudices the lymphatic circulation. Some workers believe the Streptococcus to be more important in producing lymphangitis than the worms themselves. Any foot sepsis requires early and vigorous treatment with antimicrobial drugs. Tinea infections should be eradicated. Banocide therapy is often given in elephantiasis on the grounds that it may prevent further lymphatic damage, but clinical improvement is seldom observed.
A variety of surgical operations have been devised to remove the edematous subcutaneous tissue from the leg, scrotum, and breasts. Success depends on the type of operation and the skill of the surgeon. In scrotal elephantiasis care must be taken to preserve the testicles. Hydroceles can be treated by the injection of sclerosing agents. Chyluria of bladder origin can be terminated by fulgurating the leaking bladder lymphatics. Renal chyluria is best left alone, although in the past kidneys have been wrapped in cellophane with the subsequent production of renal hypertension.
Prevention of Wuchereria bancrofti .
Diethylcarbamazine, 3 mg. per kilogram per month for 12 to 18 months, has been effective in mass treatment for preventive purposes. Residual DDT or dieldrin is effective against many of the mosquito vectors, and systematic destruction of mosquito-breeding sites has also met with success. Biologic control of mosquito vectors is receiving intensive field trials, but thus far they have not resulted in methods for mass application.