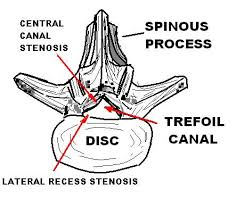
Here are Types of Spinal Injuries are being discussed.Spinal diseases often cause pain when bone changes put pressure on the spinal cord or nerves.
The Cervical Spine.
Forced flexion of the cervical spine often compresses the vertebral bodies, dislocates a vertebra forward on the one below, and interlocks the articular facets. Either the squeeze between the upper lamina and the lower body or displaced fragments of bone or intervertebral disc then compress the spinal cord. A prolapsed intervertebral disc does not usually damage the cord in a flexion injury unless the force is sufficient to cause a fracture-dislocation as well.
Flexion injuries
Its tend to block circulation in the branches of the anterior spinal artery as the result of either direct pressure or injury to the radicular or vertebral arteries in the intervertebral foramen. The resulting ischemic injury is most severe in the central portion of the spinal cord. Actual thrombosis of the anterior spinal artery is rarely observed.
Hyperextension of the neck, on the other hand, buckles the ligamentum flavum forward, pinching the cord, especially if an arthritic spur bridges the interspace anteriorly. Several centimeters of the central portion of the cord can be damaged by such an injury even though roentgenograms of the spine remain normal. The upper limbs are left weaker than the lower, and a variable loss of sensation occurs with relative sparing of touch, position, and vibration sense. Bleeding into the central cord (hematomyelia) may complicate the injury and has similar clinical effects.
Patients with injury to the cervical spine must be handled carefully to prevent an unfavorable shift of the fracture-dislocation from further damaging the spinal cord. A conscious patient usually gives warning of his plight, but the possibility of an unstable spine is easily overlooked if the patient is unconscious. A gentle pull on the head in line with the spine is advisable to keep traction on the neck whenever the patient is moved.
You Must Know The Most Common Types of Spinal Injuries
Spine boards to which the head and trunk can be strapped commonly are used to protect the spinal cord when removing a patient from a wrecked automobile. If one is not available, a bulky wrapping about the neck which supports the chin and occiput will help reduce motion that might be dangerous. A firm board or a door makes a better litter than a sagging canvas stretcher that flexes the neck. Roentgenograms are best obtained ’ on the litter to avoid the manipulation of a transfer to the x-ray table.
The primary treatment of fracture-dislocation of the cervical spine is traction with tongs or wires inserted in the skull to achieve and maintain the reduction. The pull should be in the line of the spine, and weights exceeding 30 pounds should be avoided to prevent a sudden shift from causing further damage.
After reduction is obtained, traction can be continued for six weeks, following which the patient is ambulated in a collar that is worn for three months. An acceptable alternative that shortens the period of immobilization is to perform an operation at which loose fragments of bone and disc are removed and the vertebral bodies fused anteriorly. Atlantoaxial dislocations are characteristically unstable and are appropriately treated by early fusion of the first three cervical vertebrae.
The Thoracolumbar Spine.
Hyperflexion in a fall characteristically causes compression of one or more vertebral bodies between T-12 and L-3. Unless neoplasm or osteoporosis has softened the bone, a heavy direct blow is needed to fracture the mid thoracic vertebrae.Hyperextension, plaster jackets, and operation were formerly used in an often futile effort to restore a normal roentgenographic appearance to the fractured spine. At present the deformity of a stable, fracture is accepted and treated by bed rest until the pain subsides; this is followed by progressive ambulation. The occasional unstable fracture-dislocation requires open reduction and fusion.
Surgical Decompression.
Whether surgical decompression restores function to a traumatized spinal cord is a matter of controversy. Almost no patient with a complete loss of motor power and sensation that persists more than 24 hours ever regains much useful function regardless of treatment. On the other hand, if a trace of motion or persistent sensation confirms that the cord has been only partially interrupted, surprising improvement may take place and may continue as long as two years, even without surgery.
All agree that the rare patient who shows progression of the neurological defect after an injury should have a decompression operation. Surgical debridement and closure prevent a spinal fluid fistula in open fractures, and possibly damaged nerve roots of the cauda equina benefit from decompression. At the present time many patients with fracture dislocation of the cervical spine are operated upon by the anterior approach to achieve decompression of the cord and fusion of the vertebral bodies. The results are difficult to assess because of the relatively good prognosis without surgery when the damage to the cord is incomplete, and a conservative approach is usually justified.