Trichinosis is a self-limited infection of the intestine (by the adult parasite) and of the striated muscle (by the larvae) produced by a small nematode, Trichinella spiralis. The same animal host thus acts as both the final and the intermediate host, harboring the adults temporarily and the encysted larvae for long periods. When infected meat containing larvae is ingested, these larvae are released into the upper small intestine by the action of digestive juices. They become adult in five to seven days, the males and females mate, and the fertile female begins to deposit larvae into the mucosa.
These larvae pass into the circulation through the hepatic and pulmonary filters, and are carried to all parts of the body. They burrow into the muscles and encyst and complete their development in striated muscle. In other tissues such as the myocardium, brain, and eye, the larvae disintegrate and are absorbed. Among the muscles heavily parasitized are the diaphragmatic, masseteric, intercostal, laryngeal, extraocular, nuchal, pectoral, deltoid, gluteus, biceps, and gastrocnemius. A total of 1500.larvae are liberated by each female worm, usually in four to eight weeks but up to 16 weeks, after which the females die.
Larvae attain a size of 0.4 by 0.025 mm. in a cyst in the muscle by the thirty-fifth day. The capsule is complete in three months, and calcification occurs within six months to two years. Recent evidence suggests that there may be strain differences in relation to host susceptibility. The parasite is chiefly found in man, hogs, rats, bears, foxes, walruses, dogs, and cats, but any carnivorous or omnivorous animal may be infected.
Epidemiology of Trichinosis.
Generally of worldwide distribution, the parasite has not been reported from the islands of the Pacific or Australia. It occurs more frequently in the Northern Hemisphere than in the tropics. It is common in Europe and the United States. Fatal cases have recently been described from Kenya and Chile. It is rare east of the Suez Canal. In the United States there has been a marked reduction in the incidence of the infection, owing to laws requiring the cooking of garbage fed to hogs, storage of meat at low temperature, and education of the public resulting in thorough cooking of pork.
Until quite recently, trichinosis was relatively common in New York City, as pork was being obtained from garbage-fed hogs in New Jersey. However, hog-rearing in this way has substantially declined. Pigs become infected by eating infected meat and occasionally infected rats. Rats are infected in the same way. One of the main methods of transmission is in sausages, wursts, or hamburgers in which the beef is diluted (or actually contaminated in mechanical grinders) with a little pork. Infections from bear and walrus meat have been reported, The low incidence in the tropics is probably due to the fact that meat of any kind is a luxury to many people. Hindus, Jews, and Moslems eschew pork, and the Chinese cook it very well.
Pathology and Pathogenesis.
Three to four days after invasion of the muscle, the fiber becomes edematous, loses its cross striations, and undergoes basophilic degeneration. The nuclei increase in number and size, and there is interstitial inflammation around the muscle with a chronic inflammatory cell infiltrate. The severity of the disease depends on the adult worm load, the age of the patient, and the degree of host resistance as well as the numbers of organs involved.
In the heart a focal interstitial myocarditis may occur. Acute nonsuppurative meningitis may be associated with larvae in the cerebrospinal £ Larvae may cause lesions in the chord mil retina.
Trichinosis Clinical Manifestations.
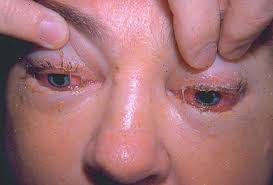
The clinical picture can be divided in different stages in a symptomatic infection . From the (sewesrm to the fourteenth day larviposition begins, and muscle penetration commenced Trie is usually associated with an irregular pers serai fever (100 to 105° F.), urticarial rash, and occasionally respiratory symptoms in the form of and bronchospasm. Muscle pains become prominent and unusual, but the characteristic physical signs are bilateral orbital edema and subungual hemorrhages. A severe infection may result in death four to eight weeks after infection from toxemia, secondary pneumonia, myocardial failure, or trichinosis encephalitis. Severe muscle involvement may render breathing, masticating, swallowing, or locomotion painful. An eosinophilia beginning seven days after the infection may rise to very high levels (70 per cent) and persist for months. Serum transaminases are also elevated in the invasive stage.
Diagnosis and Differential Diagnosis of Trichinosis.
Although the rising eosinophilia together with a suggestive clinical picture leads one to suspect this diagnosis, it is proved by finding the larvae in a muscle biopsy. This should be done in the fourth week of infection when a small piece of muscle is removed from the deltoid or gastrocnemius. Crushed between two microscope slides and examined under the low-power objective of the microscope, the living coiled larvae can be seen. In light infections when the direct examination is negative, the biopsy specimen can be incubated overnight in an acid-pepsin mixture and the centrifuged deposit examined for larvae.
Calcified cyst and calcified larvae represent older infections, as calcification usually takes 18 months, but the larva may live inside the calcified cyst for many years. Calcified cysts appear as tiny white spots in fresh muscle, but are too small to be detected radiologically.
A variety of serologic tests are available. .
The bentonite flocculation test is as sensitive as the complement-fixation test and much easier to perform. It is usually positive four weeks after infection, but may be present earlier. A change from a negative to a positive test during the illness is significant. The indirect fluorescent antibody test detects some infections at an earlier stage. Few Other parasitic infections are associated with such persistent fever or generalized muscular aches and tender muscles. Polymyositis of non parasitic etiology may present like this and be associated with eosinophilia. Periarteritis nodosa may also mimic trichinosis.
Solid Treatment of Trichinosis.
Patients with symptomatic trichinosis should be confined to bed and given a smooth high-calorie, high-protein diet. Congestive cardiac failure should be searched for and, if present, should be treated. Mild analgesics can be given for the muscle pain. Anti-inflammatory steroids (prednisolone, 5 mg. three times daily). relieve fever, edema, afid muscle pain in severe acute cases but are said not to affect the adult worms’ fecundity or the number of larvae settling in the muscle. In patients with central nervous system involvement this effect of steroids is dramatic.
Thiabendazole, in a dose of 25 mg. per kilogram of body weight for five to seven days, has also produced a marked resolution of the symptoms of fever and muscle pain, but living larvae have still been recovered on muscle biopsy after much larger courses of the drug. In severe infections the use of corticosteroids and thiabendazole may be life-saving, but when the parasite load is not considerable, the prognosis is good even without treatment.
Prevention of Trichinosis.
The ultimate prevention of trichinosis is dependent on its elimination in hogs, and the incidence in these animals can be greatly reduced by heat-sterilizing garbage. Freezing meat at —32: C. for a few hours (or at 15 to 30° C. for several weeks) kills larvae, as does gamma radiation of the meat. Pigs fed on a diet containing 0.1 per cent thiabendazole fail to incubate T. spiralis :n challenge. Routine meat inspection does not detect the infection, and serologic and skin tests on pigs have not been helpful in detecting infected animals. The chief safeguard at present is the thorough cooking of pork at 140° F. for 30 minutes for each pound of meat.
Conclusion
Trichinosis, caused by Trichinella roundworms, is a potentially serious infection that can be prevented with proper food handling and cooking practices. Additionally, early diagnosis is crucial for prompt treatment and to avoid complications. By following the preventive measures outlined in this article, you can minimize the risk of trichinosis and protect your health and well-being.