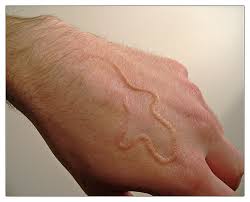
Cutaneous larva migrans is considered at this point because it’s most common cause is Ancylostoma braziliense, although it may be produced by a variety of other helminths. It is characterized by an erythematous, serpiginous, intracutaneous track or burrow, the anterior end of which is observed to migrate at the rate of 1 to 2 cm. per day. There is often intense irritation, and secondary infection may result from scratching. This migration is due to the infective larva of A. braziliense (the cat and dog hookworm), which does not viscerally in man but wanders around in the skin. This migration may last for 2 to 50 weeks before the larva dies. Rarely some larval reach the lungs, causing high eosinophilia and patchy pulmonary infiltration.
Patients are often infected by lying on beaches contaminated by dog or cat feces. The feet, legs,and hands are the most common sites, and the appearance of the lesion is usually diagnostic. It is virtually impossible to remove the larva from the skin.
Ancylostoma braziliense is found in the southern United States, Central America and tropical South America, as well as in tropical Africa and parts of the Far East, especially the Malay peninsula. There have been several reports of the worm maturing in the gut of man and eggs appearing in the feces, so there is not an absolute host specificity. Two other dog hookworms, Uncinaria stenocephala and Ancylostoma caninum, can produce similar lesions. Occasionally the ground itch of the two common human hookworms may persist and resemble creeping eruption in immune subjects.
The larva migrans track of Strongyloides ster-coralis tends to be a short line, erythematous and rapidly moving (larva currens). Rodent Strongyloides may produce similar lesions but no mature worms. A form of myiasis with the horse bot fly maggot (Gasterophilus) can produce a larger deeper migrating form of cutaneous larva migrans.
Treatment of Cutaneous Larva Migrans
Thiabendazole by mouth, 25 mg. per kilogram per day for two days, is usually effective. If not, the dose can be doubled and repeated. Alternatively, the advancing end of the burrow can be treated with topical thiabendazole sprinkled on elastoplast or in a cream containing 15 per cent thiabendazole powder in a hydrosoluble base. This drug has completely superseded the other, more unsatisfactory treatments such as ethyl chloride spray and Hetrazan.
Cutaneous Larva Migrans (CLM) is a skin condition caused by the larvae of certain species of hookworms, often found in cats and dogs. The condition primarily affects people who come into contact with soil or sand that is contaminated with animal feces containing the hookworm larvae. Here’s a tabular format guide explaining how Cutaneous Larva Migrans works:
| Stage | Description |
|---|---|
| Exposure | Person comes into contact with contaminated soil or sand, typically through bare feet or skin. |
| Penetration | Hookworm larvae in the contaminated material penetrate the skin. |
| Migration | Larvae migrate under the skin, causing visible, itchy trails or tracks. |
| Symptoms | Itching, red lines, and skin eruptions occur. The trails may move as the larvae travel. |
| Diagnosis | Based on clinical appearance and history of exposure. Skin biopsy may be used in uncertain cases. |
| Treatment | Antiparasitic medications, such as albendazole or ivermectin, are typically prescribed. |
| Prevention | Avoiding direct skin contact with potentially contaminated soil or sand, wearing protective footwear. |
It’s important to note that CLM is self-limiting in humans as the larvae cannot complete their life cycle in a human host. However, treatment is often sought due to discomfort and to prevent secondary infections.
Conclusion
Cutaneous Larva Migrans may be an unwelcome visitor, but with the right knowledge and precautions, you can reduce your risk of encountering this parasitic infection. By protecting yourself with proper footwear, practicing good hygiene, and being mindful of your surroundings, you can enjoy the outdoors with peace of mind. If you suspect you may have CLM, seek medical attention promptly for appropriate diagnosis and treatment. Stay informed, stay protected, and enjoy the great outdoors to the fullest!