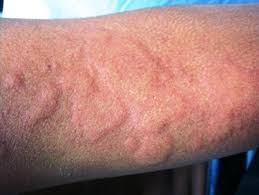
Hives Also known as Urticaria, is an eruption of the skin characterized by elevated, erythematous, sharply demarcated wheals, usually intensively neuritic, lasting hours to days hut often recurrent for weeks and sometimes years.
Etiology And Pathogenesis of Hives
The characteristic lesion is produced by capillary dilation in the dermis, leading to loss of fluid into the tissues. Swollen collagen bundles, widening of the dermal papillae, and flattening of the rete pegs are seen microscopically. It is useful to divide the causes into immunologic, paraimmunologic. and nonim-munologic categories.
By far the most common immunologic cause of acute hives is food allergy. In this circumstance, vasoactive mediators such as histamine, kinins. and slow-reacting substance of anaphylaxis (SRS-A are released from mast cells, basophils, and other tissues, producing capillary dilation The release of mediators i* typically due to interaction of antigen with circulating, or fixed, reaginic antibody, usually of the IgK variety This antibody can be passively transferred by the serum of an affected individual to the skin of a volunteer. A wheal is produced at the transfer site upon ingest ion of the offending food antigen. This is the classic Prausnitz-Kustner iPK reaction Reactions of IgK antibody with antigen are not complement dependent and produce no vascular necrosis. Complement-dependent IgG-antigen interactions may also cause mediator release by cytotoxic action on mediator-containing cells.
These reactions may be produced diator-containing cells. These reactions may be produced by antibodies directed against cell antigens, such as isohemagglutinins, and may also be due to antibodies directed against foreign antigens in which the antigen or the complex ia passively affixed to the cell surface. The urticaria of serum sickness isee Ch 711 is such an example The most frequent route of antigen presentation in the production of acute urticaria is oral ingestion Inhalation uncommonly produces hives, and occasionally contact with ullergenon the skin may suffice People sensitive to animal dander often report that contact with the furor saliva of the animal may cause hives; patients allergic to bees may develop hives of the lip* and mouth upon contact with honey.
The “paraimmunologic” causes are likely to involve similar mechanisms to those of the first category, but the relationship of the antigens and antibodies involved is less apparent. Infection with viruses, bacteria, and fungi may present with hives, hepatitis is a common example. Intestinal parasites, particularly the roundworms, are often associated with luves and cosinophilia. Bites of common insects such as mosquitoes, bedbugs, lice, and other biting insects may produce not only local manifestations but generalized urticaria.
Neoplastic diseases, particularly lymphomas of the Hodgkin’s variety, and the myeloproliferative diseases are commonly associated with hives. Finally, in the paraimmunologic category are the diseases in which immune complexes have been demonstrated and are thought to play an important etiologic role. In this group, hives are most often associated with systemic lupus erythemutosu* and derma-tomyosilis, hut tin- palpable purpura of leukocytocla»tic angiitis lllenoch-Schonlein purpura) may first appear ax urticaria and then become purpuric.
The nonimmunologtc causes of urticaria include physical stimuli such a* cold. heat, actinic energy tsolar urticarial. and pressure. Cold urticaria may he a familial or sporadic disease in which areas exposed to cold develop urticarial wheals. In about 50 per cent of the sporadic cases, a factor in scrum is capable of “sensitizing” normal skin so that a wheal develops when an ice cube is applied to the site. Cold urticaria may be symptomatic of an underlying systemic disease: multiple myeloma, cryoglobulinemia, and syphilis have been reported. The mediators responsible for cold urticaria are presumed to be similar to those released by allergic reactions, but the mechanism of release remains unclear.
Solar urticaria is produced by two spectra of actinic rays of 3100 to 3700A and 4000 to 5000A in wavelength. Marked sun exposure in a sensitive individual has led to generalized vascular collapse. Urticaria to sunlight can be passively transferred by serum from individuals who are sensitive to the lower spectrum The mechanism of mediator release is unknown but. unlike cold urticaria, treatment with drugs and barrier creams is quite effective (see below I.
Certain drugs und chemical compounds have the capacity to cause mast cell degranulation directly, resulting in mediator release without an antigen-antibody reaction. Surface-active materials such as saponin, highly negatively charged molecules like polylysines, and manv drugs share this property. Common drug examples are morphine, quinine, polymixin B. curare, decholin, hydralazine, and meperidine N’onimmunologic release of histamine may lie the basis of many “drug reactions” which have failed to yield immunologic mechanisms such as the rare reactions to radiographic contrast agents which are iodinated organic compounds Indeed, the warm “glow” produced by good brandy is prohably more a factor of mediator release than alcohol content, as any ethanol sampler can attest.
A special form of urticaria which coiui»t»of*mall, al-most papular, wheals surrounded by u large axon flare is called cholinergic urticaria. Affected individuals will produce u similar eruption when injected with small amounts of mecholyl or acetylcholine The mechanisms are obscure, but clearly emotional stress, exposure to heat, such as a warm bath, or exercise may bring out the eruption.
Urticaria pigmentosa, or systemic mastocytosis, is due to infiltration of the skin by mast cells: it is believed to be a true neoplasm of very slow growth in which the chemical manifestations are much more distressing to the patient than the invasive ones. Areas of infiltration are marked by freckle-like hyperpigmentation which, upon stroking, will produce a typical linear bumpy wheal, because the skin between the accumulation of mast cells does not urticaria.
Chronic urticaria implies recurrent lesions for a period of six weeks or more. The clear causal relationship of certain foods to acute urticaria has led to the assumption that the chronic form is due to an extended exposure to an unidentified allergen or urticator. Investigation of such patients yields a single causal factor in very few, and the bulk of these patients defy elucidation of a specific etiologic factor Many writers have emphasized psychologic factors in chronic urticaria, supporting their arguments with numerous cases of acute urticaria in rwponftc to a specific stress a heavy date, un important examination, or the like. Although these factors must play some role, their magnitude in a particular patient in very difficult to assess.
Clinical Manifestations of Hives.
Typically, the wheal is I to 5 cm in diameter, often irregular, with a blanched center (“target” lesion • and surrounding erythema. The individual lesions are evanescent, often fading within hours. Successive crops appear for the duration of the disease. The lesions tend to appear at pressure points-e.g., the belt line, the brassiere straps, or the garters. Rarely are the soles and palms affected; but when they are, the patient may complain of difficulty in walking. Pruritus is common and sometimes so severe that the patient cannot wait to get home and fling off his or her clothes. When urticaria is due to a single exposure to a food or drug, it usually appears within minutes. An ingestant taken more than 24 to 48 hours before onset is rarely the cause. Occasionally summation of two allergic stimuli may be responsible: e.g., some patients may eat frozen strawberries in winter with impunity, but during the pollen season the same strawberries will cause hives.
Treatment of Hives.
Acute or sporadic urticaria usually responds well to antihistaminics such as brompheniramine iDimetane), 4 mg every four hours, or tripelennamine • Pynbenzaminei 50 mg every four hours. If the patient is in acute distress, 0.3 ml of 1:1000 epinephrine suhcu-taneously will often provide relief until the antihista-mimcefTect is apparent In severe or unresponsive cases of sporadic urticaria, four days of prednisone, 40 mg per day may be necessary and very helpful.
In chronic urticaria the cause is randy evident and therefore hard to remove. Most patients have been treated with antihistaminics without benefit. The use of a rigid elimination diet may not only remove hidden allergens, but more likely may also remove foods such as spices which are direct releaser* of histamine. In addition to the elimination diet, liberal doses of brompheniramine (Dimetane), 8 mg every four hours, and hydroxyzine. 10 to 25 mg three times a day, are helpful. After a period of relief, cautious reduction of the drug regimen and addition of selective foods in groups, such as eggs, milk, and milk products, one at a time every three to four days, will often result in cessation of symptoms The result is frequently a grateful patient on a full diet; the doctor, however, remains perplexed.
Cold urticaria is often refractory to treatment with all the agents mentioned above, and often the patient has to adjust his life style to avoid the cold. In contrast, solar urticaria is readily treated with barrier creams that filter out the actinic energy of the appropriate wave length Hydroxychloroquine U’laquenil), 200 mg. once daily or even twice a week, may protect a sensitive per son who anticipates sun exposure.
Hives CAUSES:
The ‘ acute urticaria is often caused by an allergy to food (fish, shellfish, peanuts, strawberries, spices, etc.), With preservatives and food coloring, to pollen or dust, drugs (eg. Antibiotics, anti-inflammatories , vaccines and anesthetics). It can be caused by intestinal parasites (ascarids and pinworms), insect bites, irritations from fabrics (silk, wool) or dyes.
Finally we find acute hives from stress, stress and physical causes (heat, cold, pressure, vibrations, water, ultraviolet rays). L ‘ chronic urticariahowever, in 60% of cases it is an autoimmune disease, that is caused by the formation of antibodies directed against the skin. This causes the release of stinging substances that cause chronic symptoms as a reaction. Among other causes of chronic urticaria: connective diseases (eg lupus erythematosus or scleroderma), in which cutaneous symptoms are associated with joint pain, fever, or respiratory and digestive disorders.