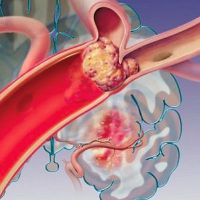
Fat embolism is the obstruction of blood vessels by fat droplets that most often happens after fractures of long bones, such as bones of the legs, thighs or hips.It may also arise in the postoperative period of orthopedic surgeries or procedures such as liposuction.
Fat embolism is the obstruction of blood vessels by fat droplets that most often happens after fractures of long bones, such as bones of the legs, thighs or hips, but which may also arise in the postoperative period of orthopedic surgeries or procedures such as liposuction.Fat embolism of the lungs results from the impaction of particulate fat globules in the pulmonary circulation. After long bone fractures most patients develop fat embolism, but most do not develop the fat embolism syndrome, which includes the presence of at least one of three major symptoms: respiratory insufficiency, and cerebral symptoms.
For example, microscopic fat embolism can be detected in the femoral vein draining the operative site in virtually all patients undergoing a total hip replacement, but none of the patients develop the fat embolism syndrome. With fractures of the pelvis or long bones in the legs only 2 per cent of patients develop the overt fat embolism syndrome, but approximately half develop transient hypoxemia, often with thrombocytopenia, suggesting a subclinical fat embolism syndrome.
PATHOGENESIS of Fat Embolism
The pathogenesis of the fat embolism syndrome may be more complicated than the simple physical occlusion of arterioles by fat globules released from marrow. It may relate to the hydrolysis of the triglycerides by lipoprotein lipase, releasing free fatty acids which are considerably more toxic to the endothelium than the triglycerides themselves. The concentration of free fatty acids may be higher in the immediate vicinity of fat globules obstructing pulmonary arterioles or capillaries, producing additional chemical injury, complicated by platelet and fibrin thromboses.
Since many patients with fractures develop fat emboli, why do only a few develop the fat embolism syndrome? There is evidence that patients who develop the syndrome are constitutionally different from people with similar degrees of trauma who do not; they have significant abnormalities of carbohydrate and lipid metabolism and of coagulation, increased capillary fragility, and abnormal neurohumoral regulation in response to exercise stress. In particular, they have a higher incidence of elevated blood sugar or diabetic history and significantly higher levels of beta lipoproteins. Both the diabetic state and familial elevations of beta lipoproteins have been shown to be associated with abnormalities of platelet aggregation.
Main causes of Fat Embolism
Fatty embolism can be triggered by situations such as:
- Fracture of bones , such as femur, tibia and basin, after an auto accident or fall;
- Orthopedic surgeries , such as knee or hip arthroplasty;
- Plastic surgery , such as liposuction or fat fillings.
Fat Embolism CLINICAL FEATURES.
In the typical patient with the fat embolism syndrome tachycardia of 140 beats per minute, tachypnea of 30 to 40 breaths per minute, and fever up to 39°C are noted two or three days after a fracture. The patient may or may not appear cyanotic, rales may be heard, and petechiae are common, particularly around the axillary folds, the neck and upper chest, and the conjunctivae or optic fundi. The patient often develops restlessness or increasing irritability, which may progress to delirium or coma. Xot every patient has all these findings. A reasonable approach to the diagnosis is to insist on one major feature and four minor features, along with demonstration of fat macroglobulinemia and hypoxemia.
The major features of the fat embolism syndrome are (1) respiratory insufficiency, (2) cerebral involvement, and (3) petechial rash. The minor features are (1) pyrexia, (2) tachycardia, (3) retinal changes, (4) jaundice, (5) renal changes, (6) anemia, (7) thrombocytopenia, and (8) elevated sedimentation rate. Fat globules can be demonstrated in venous blood with a crvostat technique or by filtering serum through an 8 micron MiUipore filter and staining the filter for fat with a Sudan IV stain. In 100 patients with the fat embolism syndrome, the initial findings on admission were cerebral symptoms (usually drowsiness or confusion), 34 per cent; tachycardia and pyrexia, 29 per cent; respiratory dysfunction with dyspnea, tachypnea, or hemoptysis, 20 per cent; and petechial rash, 17 per cent. Recover)’ was complete in 77 patients and partial in seven. Sixteen patients died, eight from the fat embolism syndrome and eight from the trauma itself.
Three different syndromes of fat embolism have been described: (1) In the hyperacute response, death is due to systemic embolization of the brain or coronary arteries. (2) In the classic response, roentgenographic findings in the chest are variable, ranging from a normal pattern or patchy densities to linear streaks radiating out from the hilar region. About a third of the patients show frank pulmonary edema, yet their hypoxemia may be fully corrected by increasing the fraction of inspired oxygen to 40 per cent. Mild abnormalities of the prothrombin time and activated partial thromboplastin time (APTT) and platelet counts occur. (3) The third syndrome is the adult respiratory distress syndrome. These patients have acute pulmonary edema demonstrated radiographically and require an increase in Fi^ to 60 per cent to correct hypoxemia. They have evidence of disseminated intravascular coagulation with thrombocytopenia, prolonged prothrombin time and APTT, lowered fibrinogin concentration, and elevations of fibrin degradation products. At autopsy, intra-alveolar hemorrhage, infiltration of macrophages and mononuclear cells, and platelet and fibrin aggregation within multiple capillaries and arterioles are found.
Fat Embolism Treatment.
The most important aspect of treatment is oxygen therapy. If more than 50 per cent oxygen is required, intubation of the patient is advisable so that positive end-expiratory pressure (PEEP) can be used. An optimal level of PEEP can usually be found that allows greater delivery of oxygen to the tissues at a lower inspired oxygen tension than without PEEP. Early treatment with corticosteroids, although unproved, may be beneficial. For example, when massive doses of methvlprednisolone (30 mg per kilogram intravenously at eight-hour intervals) are used prophylactically in patients at high risk for fat embolism syndrome, there is significant improvement in the artenal oxygen tension and prevention of abnormalities of coagulation tests and platelet counts.
PROGNOSIS OF Fat Embolism
The prognosis for the fat embolism syndrome is better than for most causes of the adult respiratory distress syndrome. In fat embolism syndrome the mortality rate is about 8 per cent, compared to about a 50 per cent mortality rate for most other causes of the adult respiratory distress syndrome.