The term Cutaneous leishmaniasis or “oriental sore” has many synonyms, such as Aleppo, Baghdad, or Delhi boil; bouton d’Orient; bouton de Biskra; chiclero ulcer; forest yaws. It is applied to an infection characterized by cutaneous granulomas with a tendency to ulceration and chronicity.
Oriental sore is prevalent in many tropical and subtropical regions in both Eastern and Western Hemispheres. It occurs in Asia, especially in the Middle East, in the Mediterranean littoral, in southern Europe and the Mediterranean islands, in Africa, and in every country in Central and South America except Chile.The agent is Leishmania tropica, which is morphologically identical with L. donovani and L. brasiliensis.
Experimental and epidemiologic evidence indicates that sandflies are natural vectors of the disease, particularly Ph.lebotom.us papatasii and .P. sergenti in the Near East and P. macedonicum in Italy. Successful inoculation of man by the bite of P. papatasii has been accomplished. In Central and South America P. intermedius is generally regarded as a vector, and several other species may be concerned. In central Asia, the gerbil, a rodent, is an important reservoir. Although infection by L. tropica occurs by direct inoculation, the parasites do not penetrate the unbroken skin.
Cutaneous leishmaniasis may occur in almost epidemic form. Children are more commonly affected than adults. There is no distinctive sex incidence. A fairly solid immunity follows infection in man. This has long been the basis for deliberate inoculation of children in endemic areas, the inhabitants knowing that the induced attack confers protection against naturally acquired infection. Sites are chosen where the resultant scar will be least disfiguring.
Pathology of Cutaneous leishmaniasis
Following inoculation of the skin either through the bite of an infected sandfly or by some other means, a nodule develops that is produced by infiltration of the corium with plasma cells, lymphocytes, and large endothelial macrophages. Thinning and atrophy of the overlying epidermis often occur. Perivascular infiltration then becomes prominent and inflammatory cells more numerous. Focal accumulations of endothelial phagocytes filled with leishmania are seen.
With further progression, an ulcer develops that has a granulation tissue base and a surrounding zone of inflammation. Infiltration extends into the subcutaneous connective tissue in which reticuloendothelial cells, plasma cells, and lymphocytes are prominent. Occasional giant cells are present.
The leishmania: re often difficult to demonstrate in the fully developed ulcer and may be found only at the margin of the lesion or in scrapings from its floor. There is no general dissemination of the parasites. Ultimately the leishmania disappear, granulation tissue becomes more abundant, and healing occurs, leaving a depressed fibrous scar.
Clinical Manifestations of Cutaneous leishmaniasis.
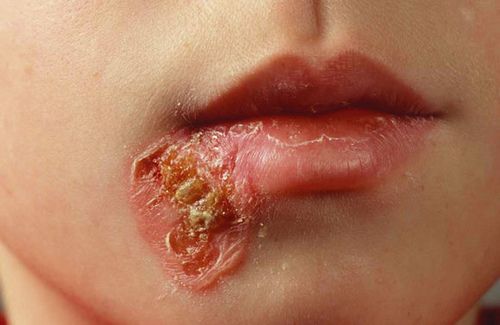
The incubation period of oriental sore may vary from a few weeks to several months. The lesions may be multiple. They appear first as slowly growing papules on an exposed skin area. As ulceration develops, they become covered with a crust that exudes a sticky secretion. On removal of the crusts, moist, freely bleeding ulcers are revealed. These ulcers are usually not deep and ordinarily vary from 1 to 3 cm. in diameter.
Secondary infection is usual and, when severe, greater tissue destruction may result. After effective treatment, or after a number of months if no treatment is given, healing occurs by granulation, and a lasting immunity is produced. In extensive multiple ulceration there may be numerous associated subcutaneous nodules that contain leishmania. A nodular or verrucous form affecting the limbs and face has been described, particularly for Venezuela and Ethiopia. It may closely resemble leprosy —many patients have been incarcerated in leprosariums — and is known as leishmaniasis tegumentaria diffusa. Numerous parasites are present in the nodule. It probably represents an unusual host response, as the leishmania skin test is negative.
Dry and moist types of cutaneous leishmaniasis have been described. In the dry type, the incubation period and duration of the lesions are long; dry papules persist for months before ulcerating. The incubation period and duration of the moist lesions are shorter; they ulcerate rapidly. Vaccination with either type apparently does not provide cross-immunity.
Diagnosis of Cutaneous leishmaniasis
The development of one or more cutaneous ulcers on exposed skin areas of the body in a region where oriental sore is known to be endemic and where sand flies are present should arouse suspicion of this condition. Definitive diagnosis depends upon the demonstration of L. tropica obtained from the lesion. In general, the longer the lesion has been present, the more difficult it is to find parasites.
Examination of the exudate will seldom be successful. Smears made from curettings of the base or the sides of the ulcer should be used, or a fine hypodermic needle introduced through normal skin may be inserted into the indurated margin of the lesion and material aspirated for preparation of a stained smear. Under sterile conditions, material aspirated from the margin of the lesion may be inoculated into NNN (Novy-MacNeal-Nicolle) medium and leptomonad forms recovered after incubation at 22° C. Bacterial contamination of cultures for leishmania may be prevented r controlled by the addition of penicillin and other suitable antimicrobials.
The other diagnostic procedures of value in kala-azar are not appropriate for oriental sore. Leishmania are not found in the blood, and anemia, leukopenia, and hyperglobulinemia are not features of this infection.The differential diagnosis of cutaneous leishmaniasis must include blastomycosis, yaws, tertiary syphilis, and lupus of the discoid type. The leishmania test is usually positive.
Treatment of Cutaneous leishmaniasis.
The tendency is for spontaneous cure with solid immunity against further challenge. Therefore, if the lesion is solitary and not on the face, all that is usually needed is the treatment of the secondary bacterial infection often found with the sore. If there are multiple lesions or if it is a disfiguring site, i.e., top of the nose, systemic Pentostam should be given in the aforementioned dose. A one-week course is usually sufficient. Infrared lamp exposure has been successful, as the organisms are very temperature dependent.