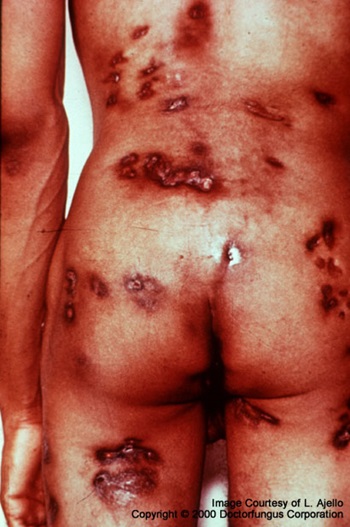
Coccidioidomycosis is a systemic fungal disease, respiratory in origin, that spreads hematogenously to skin, subcutaneous tissues, bone, central nervous system, and other organs. Severity ranges from inapparent infection to fatal outcome.
History of Coccidioidomycosis
In a series of papers between 1892 and 1898 Posadas and Wernicke described an illness characterized by severe skin lesions and widespread dissemination in a soldier from northern Argentina, hospitalized in Buenos Aires. The infection was caused by an organism they considered a protozoon. This misinterpretation was shared by Rixford and Gilchrist, who in 1894 and 1896 named the organism Coccidioides (considering it related to Coccidium) immitis Ophuls in 1900 correctly identified it as a fungus. Gifford and Dickson associated the disease they termed coccidioidomycosis with San Joaquin Valley fever, and mild disease in the majority of cases.
Etiology of Coccidioidomycosis
Coccidioides immitis is a dimorphic fungus existing in either a tissue or a saprophytic form. Arthrospores from the saprophytic phase, when inhaled by man or inoculated into animals, germinate, with the formation of the distinctive spherule measuring from 10 to 70 fi in diameter. This ruptures, releasing 10 to 200 endospores that reinfect adjacent or remote tissue. Spherules or endospores on inoculation onto Sabouraud’s glucose medium produce a cottony, aerial mycelium, composed of arthrospores (saprophytic form). Cutaneous hypersensitivity and complement-fixing antigens have been demonstrated. Mice and guinea pigs are susceptible to experimental infection.
Pathology of Coccidioidomycosis.
In early lesions the reaction about endospores is pyogenic and similar to that in pneumonias of bacterial origin. Spherules, however, induce a histiocytic reaction with giant. cells. Pulmonary lesions may progress with caseation, cavitation, pleuritis, and involvement of the peribronchial of paratracheal lymph nodes. As healing occurs, there is hyalinization of non necrotic granulomas. Solitary nodules resembling those of tuberculosis or histoplasmosis (q.v.) may result. Lesions of other organs are also both suppurative and granulomatous.
Clinical Manifestations of Coccidioidomycosis.
In 60 per cent of infections no illness suggestive of coccidioidomycosis can be identified. In the remaining 40 per cent an influenza-like illness can be diagnosed retrospectively (15 per cent), or a more severe illness causes the patient to see his physician at the time (25 per cent).
Primary Pulmonary Form of Coccidioidomycosis.
The incubation period varies from 7 to 28 days depending, probably, on the severity of exposure. The prototype of this illness, “valley fever,” is well characterized by headache, backache, fever, malaise, cough, fatigue, and pleuritic pain, all resembling those of j-jt uenza. Valley fever differs, however, in the greater frequency of summer illness, erythema nodosum, arthritis, and eosinophilia.
The appearance of the chest film is dependent on the severity of illness and may show peribronchial infiltration, patchy pneumonitis, thin-walled cavities, or hilar adenopathy’. Laboratory studies reveal a leukocytosis, an increase of the erythrocyte sedimentation rate, and the transient appearance of circulating antibodies. Pleurisy with effusion and pericarditis are occasionally encountered involvement also are seen. The coccidioidin skin test is usually negative, whereas the complement-fixing antibody titer generally rises.
Benign Residual Form.
Two to 8 per cent of patients are left with residual cavitary disease in the lungs. Hemoptysis, rupture with pneumothorax, and pleuritis with or without effusion are occasional complications. Solitary nodules (cocci-dioidomas) measuring from a few millimeters to 5 cm. in diameter resemble those of tuberculosis or histoplasmosis in the frequency of calcification, occasional excavation, and refilling. Diffuse pulmonary fibrosis is a common but not clinically important manifestation of residual disease. Bronchiectasis occurs with greater frequency in endemic areas and may be related to past infection with this fungus.
Primary Extrapulmonary Form.
This is a rare form of disease that follows traumatic implantation of the skin or subcutaneous tissue. It is characterized by a local lesion with regional lymphadenopathy.
Diagnosis of Coccidioidomycosis.
The diagnosis of coccidioidomycosis is proved by the isolation of the fungus in culture or by the microscopic demonstration of characteristic spherules in properly stained tissue sections. Skin tests and serologic studies as described under Histoplasmosis (q.v.) have been more helpful in coccidioidomycosis, though often negative in early disease.
Coccidioidomycosis should be suspected as the cause of any febrile or pneumonic process in a patient living in or recently returned from an endemic area: Disseminated subcutaneous and osseous forms of the disease must be differentiated from bacterial cellulitis and osteomyelitis. All forms of the disease may resemble tuberculosis and other fungal infections, especially histoplasmosis.
Treatment of Coccidioidomycosis
Amphotericin B, the only antifungal drug of demonstrated efficacy in coccidioidomycosis, is indicated in all cases of disseminated disease and should be administered as described for histoplasmosis (q.v.). In general, it is demonstrably less effective, but larger doses have been associated with dramatic responses in patients desperately ill with meningitis and osteomyelitis. In coccidioidal meningitis, intrathecal administration is necessary two to three times weekly in dosage of 0.5 to 1.0 mg. in 1 ml. of glucose solution, diluted with 5 to 10 ml. of cerebrospinal fluid and injected slowly. A cisternal rather than lumbar site of injection seems preferable. Even with these precautions, side effects of pain and paresthesias are not uncommon.
In benign residual coccidioidomycosis, complications of cavities are indications for pulmonary resection. Amphotericin B therapy pre- and postoperatively is a reasonable, though apparently not always necessary, adjunct to surgery. Coccid-idiomas, rarely dangerous to the patient, cannot be distinguished beforehand from malignant lesions, and surgical excision is usually necessary.Bed rest and supportive therapy are sufficient treatment for the influenza-like primary form of disease.