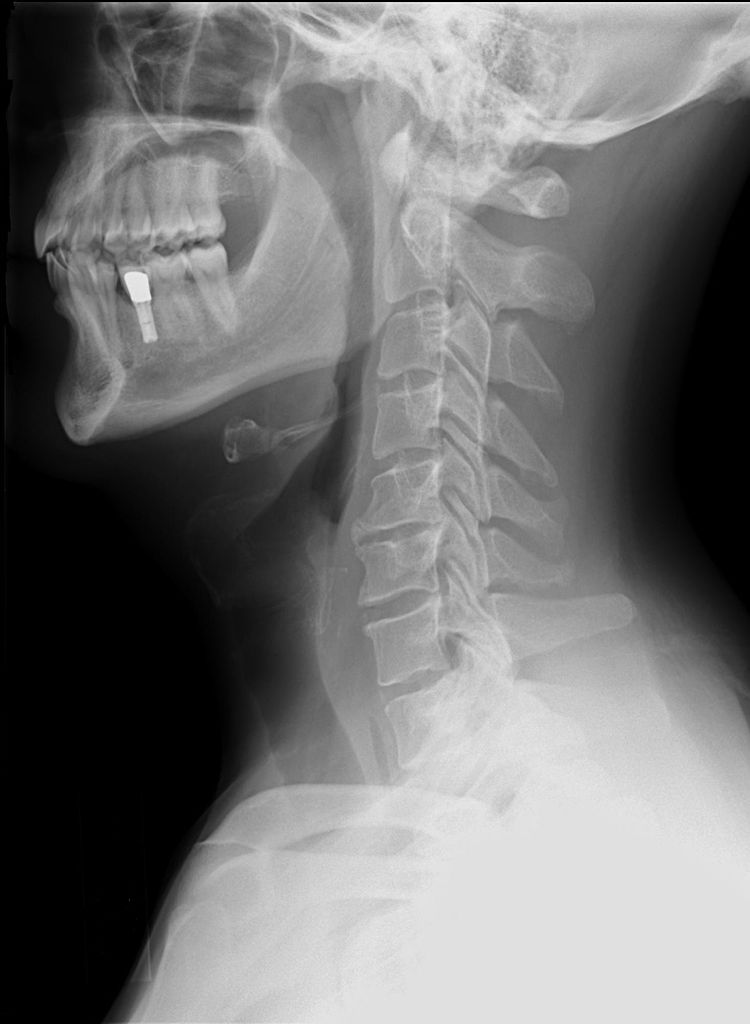
Cervical spondylosis is a chronic degenerative disease of the cervical spine and inter vertebral discs akin, to Osteoarthritis. Loss of elasticity of the disc owing to aging and causes the inter-vertebral disc space to narrow.
The anulus fibrosus consequently bulges, and may calcify to form osteophytes. Transverse osteophytic ridges diminish the anteroposterior diameter of the spinal canal, and spurs protrude more laterally into the spinal canal or encroach upon the intervertebral foramina, where they compress nerve roots or the spinal cord’s blood supply. Spondylosis is present in most persons by middle age, but spinal cord and nerve root compression occurs in only a few. More severe degrees of the arthropathy, repeated trauma, a smaller than normal anteroposterior diameter of the cervical canal, and fibrosis of the adjacent root sleeves limiting mobility of the spinal cord are all factors that hasten the development of symptoms.
Clinical Manifestations of Cervical Spondylosis.
Almost all patients are 45 years old or more. The incipient symptoms include mild restriction of neck movement or aching discomfort and paresthesias in the C-6 or C-7 distribution, often accentuated by posture and movement and difficult to distinguish from symptoms arising from muscle tension or neurovascular compression at the thoracic outlet. In more advanced stages of the disease, laterally placed osteophytes are likely to cause root pain and paresthesias, segmental weakness, and atrophy and fasciculations in one or both upper extremities.
The earliest signs of spinal cord compression may consist of a reduced perception of vibration sense in the lower extremities. Later, the stretch reflexes are increased, and extensor plantar responses emerge. With advanced spinal cord involvement, the legs become spastic and weak; paresthesias extend up the legs in socklike distribution, and loss of position sense is added to the vibratory impairment. A sensory level with change to pain and temperature sensibilities may develop on the trunk. Unless acute trauma is superimposed, the process follows an irregular course with long periods of lack of progression. Serious sphincter involvement almost never occurs.
Laboratory findings are only of partial help in diagnosis. Many patients have the roentgeno- graphic changes of cervical spondylosis, so that correlation with the neurologic changes must be made cautiously. The cerebrospinal fluid is usually normal in spondylosis, although the protein content may be raised modestly, and some patients have a partial manometric block. Pantopaque myelography establishes the diagnosis in doubtful cases by demonstrating encroachtnent of the osteophytes on the spinal canal.
Differential diagnosis includes the subacute combined degeneration of pernicious anemia, spinal cord tumor, motor system disease, and syringomyelia.
Cervical Spondylosis Treatment.
Treatment of cervical spondylosis is unsatisfactory in general. Most patients progress extremely slowly, and their neurologic deterioration halts if they are no longer exposed to trauma and if moderate traction and partial and section of the dentate ligaments may be needed.