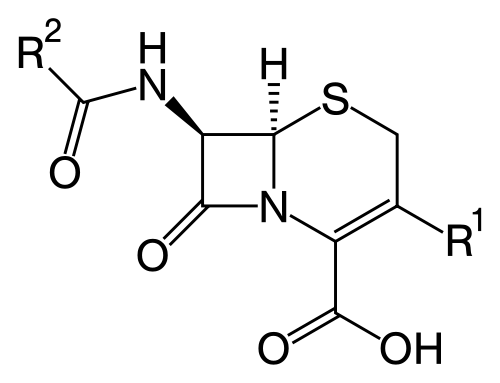
Cephalosporins are structurally related to penicillins, yet there are major differences in activity between these agents in vitro and in vivo. The first cephalosporins, such as cephalothin, cephaloridine, and cefazolin, were effective against penicillinase-producing staphylococci as well as pneumococci and streptococci (except enterococci). Additionally, they offered good activity against several important gram-negative pathogens such as £. coli, Klebsiella and Proteus mirabilis.
Despite activity in vitro, they are not effective against Salmonella and Shigella and do not penetrate the blood-brain barrier. The enormous popularity of these agents appears related to a low incidence of side effects, fairly broad coverage against community-acquired respiratory and unnary tract pathogens, and the availability of both oral and parenteral dosing. Nevertheless, these compounds have not been considered the agents of choice for any serious systemic infections.
They have been successfully used to treat patients with a history of mild penicillin type reactions, such as rash but not urticaria or anaphylaxis. With the development of newer cephalosporins the principal advantages of these older compounds (often referred to as “the first generation”) have been in the prophylactic surgical usage and relatively greater activity against penicillinase-producing Staph, aureus.
What Is Cephalosporin For?
The cephalosporins are used for the treatment of different types of infections, even serious, supported by bacteria that are sensitive to their activity:
- infections of the respiratory tract upper and lower: tonsillitis , laryngitis , laringootracheiti, tracheobronchitis, bronchitis, acute and chronic, bronchopneumonia, pneumonia, otitis, sinusitis;
- hepato-digestive infections : anogiocolitis, gastroenteritis;
- infections of the skin and tissues soft ;
- infections of the reproductive organs , of the urinary tract and of the kidneys ;
- dermatological infections ;
- infections of the blood caused by bacteria: bacteremia;
- meningitis ;
- infectious diseases of the child ;
- infections in subjects in immunocompromised patients ;
- infections of the abdomen ;
- pre , intra and post-operative prophylaxis ;
- infections of bones and joints .
The so-called “second generation” cephalosporins offer a few improvements over cephalothin and cefazolin. Cefoxitin is a compound with fairly consistent activity against B. fragilis. Cefamandole and cefuroxime lack the anaerobic spectrum of cefoxitin but have modestly improved activity against some gram-negative organisms not inhibited by the first generation, such as H. influenzae and Enterobacter species. Oral agents include cefaclor, which has greater activity against penicillinase-producing H. influenzae than cephalexin.
The newest cephalosporins (often referred to as “third generation”), or structurally related compounds such as moxalac-tam, a 1-oxy-beta lactam, have markedly enhanced activity against enteric bacteria as well as variable coverage of P. aeruginosa. These compounds are stable against the beta-lacta-mases of H. influenzae and N. gonorrhoeae and cross the blood-brain barrier in sufficient concentrations to offer effective therapy for gram-negative meningitis (with perhaps the exception of P. aeruginosa infection).
Among the agents shown to be effective in gram-negative central nervous system infections are cefotaxime, moxalactam, ceftazidime, and cefatriaxone. Several of these agents have a much longer half-life than first-generation cephalosponns, permitting dosing intervals of 8 to 12 hours. In the case of one agent, cefatriaxone, once-a-day dosing has been possible in some infections because of an 8-hour half-life. The antipseudomonal activity of these compounds is variable, and clinical data are still lacking to support the claim that these agents may be used as single agents to treat serious systemic pseudomonal infections in immunocompromised hosts. Nonetheless, newer antipseudomonal cephalosporins like cefsulodtn and ceftazidime represent some of the most potent antipseudomonal agents introduced into clinical practice, and these compounds appear to be significantly safer than aminoglycosides.
As a general rule, the increased activity against gram-negative pathogens is also coupled with relatively diminished activity against gram-positive cocci. While the gram-positive, particularly antis-taphylococcal, coverage of these agents may be satisfactory for initial therapy, serious staphylococcal disease as well as pneumococcal infection is better and certainly more economically treated with older beta-lactam agents (e.g., oxacillin, penicillin G, respectively).
These agents are also not without serious untoward effects, including the triggering of disulfiram reactions, inhibition of platelet adhesiveness, and hypoprothrom-binemia. In many patients with community-acquired and mild to moderately severe nosocomial infections, third-generation cephalosporins offer the potential of effective single agent therapy. The preliminary results in immunocompromised hosts suggest that these compounds may still be more efficacious when combined with aminoglycosides.