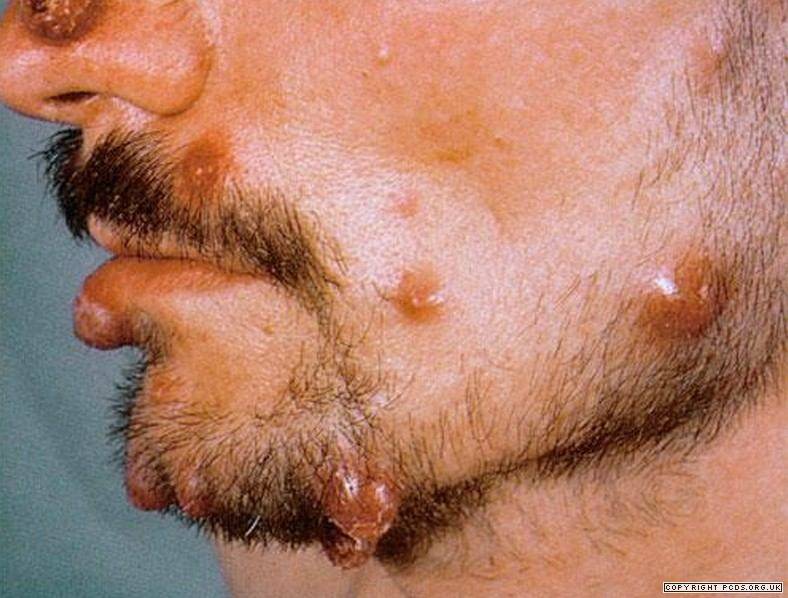
Bartonellosis is an insect-borne bacterial disease limited to South America. It is characterized by two distinctive clinical stages. The first of these (Oroya fever) presents a severe febrile infection associated with a marked anemia, bone and joint pains, bacteremia, and an appreciable mortality. The second stage (verruga peruana) is more benign and is distinguished by the appearance of a generalized eruption of hemangiomatous papules and nodules.
Etiology.
The disease is caused by Bartonella bacilliformis, a small gram-negative pleomorphic bacillus that may be cultivated readily in enriched bacteriologic media. The disease is transmitted to man by the bite of sandflies of the genus Phlebotomies, with development of the characteristic symptoms of Oroya fever after an incubation period of two weeks to three months.
Prevalence and Distribution.
Although a number of epidemics of the disease have been reported, it is more commonly seen as sporadic cases among populations of Peru, Colombia, and Ecuador, and is restricted within these countries to those who live at altitudes of 1500 to 9000 feet on both slopes of the Andes. In general, the distribution of the disease coincides with the ecologic zones supporting populations of Phlebotomus.
Epidemiology.
In Peru the disease is transmitted by Phlebotomus verrucarum, a night-biting sandfly. The biting habits of the vectors in the other countries are similar, although the species of Phlebotomus involved in transmission in the other areas are not conclusively identified. The principal reservoir of the disease appears to be man; no additional animal reservoirs have as yet been implicated in nature. Reports of cultivation of the agent from apparently healthy persons suggest that as much as 10 per cent of infections may be subclinical. Persons convalescent from the disease are known to have a low-level bacteremia for months or years, providing frequent opportunities for infection of the disease vector.
Pathology and Physiologic Responses.
In the Oroya fever stage of illness the causative organism may be found in peripheral blood smears stained with Giemsa or^rights stain reticuloendothelial cells of the viscera and lymphatics. In the blood the parasite is found both free in the plasma and adhering to the erythrocytes. The parasitization of the erythrocytes causes an increased mechanical fragility and also an increased sequestration of the cells in the spleen and the liver. A hypochromic and macrocytic anemia develops rapidly during the febrile period, erythrocyte counts decreasing within a period of only a few days to levels of one million to two million cells per cubic millimeter. The bone marrow is hyperplastic, with an abundance of nucleated erythrocytes. The pathologic findings secondary to the anemia are absent in the verruga stage of infection. The histopathology of the skin lesions is that of dilation of the capillaries and proliferation of the vascular endothelial cells that may be shown to contain the causative agent.
Clinical Manifestations of Bartonellosis.
The presenting- symptoms of patients with Oroya fever are intermittent high fever, painful muscles and joints, tender enlarged lymph nodes and the systemic symptoms and prostration of a severe anemia. These symptoms may persist from several weeks to several months in untreated patients, half of whom may die within the first three weeks of fever. If the patient survives, gradual convalescence is punctuated, after a few days to a month, by the appearance of the cutaneous lesions of the second phase of the disease.
The verrucae may persist for a month to a year in untreated persons, but mortality is negligible. Occasional patients may ex-perience only the fever and anemia without the skin manifestations, or only the cutaneous lesions without the initial fever. Although these two aspects of the infection were once thought to be different diseases, there is no doubt that both syndromes are manifestations Of infection with the same organism. The current interpretation that the skin lesions are an expression of developing immunity in the patient is supported by the observation that second attacks of the disease are exceedingly rare even in highly endemic areas and that the attacks are almost always caused by verruga rather than by Oroya fever.
Bartonellosis Diagnosis.
In endemic areas the diagnosis can usually be made on the basis of clinical findings. In the acute stage of Oroya fever both blood smears and blood culture usually reveal the presence of the agent. As the patient progresses toward the verruga stage of infection, or with treatment, the organism becomes more difficult to demonstrate.
Treatment and Prognosis of Bartonellosis.
The prognosis in the untreated patient depends upon both the nature and the severity of his infection. Mortality in the Oroya fever phase of the disease may exceed 50 per cent, particularly when the infection is complicated by concurrent attacks of malaria, amebiasis, tuberculosis, salmonellosis, or other diseases. The disease responds well to treatment with penicillin, streptomycin, chloramphenicol, and the tetracyclines. Chloramphenicol is favored by many South American clinicians because of the frequency of concurrent salmonella infections, but the risks of its potentially more serious toxicity must be weighed against the fact that the other drugs mentioned are therapeutically effective.
In general, as in the rickettsial infections, the tetracyclines are the -preferred form of antimicrobial therapy for bartonellosis. When the broad-spectrum antimicrobials have been used, oral doses of 1 to 2 grams per day have been used for a period of a week or more with excellent results. Patients become afebrile in 24 to 48 hours, and, if they receive transfusions, recover strength rapidly. Although the mortality of the verruga stage of infection is less than 5 per cent, antimicrobial therapy is desirable to hasten the disappearance of the skin lesions.
Prevention.
Control measures are directed principally against the Phlebotomus vector. Because the insect is a night feeder and moves by a series of short “hops” between surfaces, the application of a residual insecticide, such as DDT, to the exterior and interior of doorways, windows, and other avenues of entry to human habitation is effective. Where insecticide application is impracticable, bed nets or insect repellents provide significant protection. Control of breeding of the vector is difficult, but may be undertaken when it is otherwise impossible to prevent contact of the vector with man. No protective vaccine is available. Patients need not be isolated in hospital wards if the vector is absent because the disease cannot be transmitted by person-to-person contact.