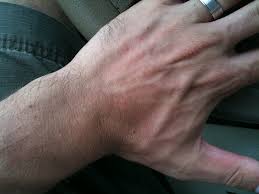
Radiation poisoning is manifested in a number of ways, depending upon the nature of the exposure. Massive radiation exposure causes injury that may be evident within minutes or days, whereas small or repeated exposure induces a response that may not be apparent for years. If the entire body or a large portion thereof is irradiated with a large dose of penetrating radiation, an acute generalized illness called the acute radiation syndrome results. If a small portion of the body is exposed to an excessive dose, a localized injury occurs perhaps with little, if any, systemic reaction.
Such localized injuries are usually named after the organ affected, e.g., radiation dermatitis, radiation nephritis, etc. Although acute radiation injuries have distinctive characteristics, the delayed manifestations or late effects of radiation injury (terms preferable to delayed radiation injury) may be indistinguishable from spontaneously occurring diseases, such as leukemia.
Etiology
Known instances of radiation poisoning in man are usually the result of exposure to radiation from radiation sources. – In peacetime, such exposures are almost exclusively medical or industrial and, in the case of late manifestations, may have occurred so long before as to have been forgotten. As knowledge of radiation hazards has been gained, it has become evident that exposure fo doses formerly thought to be harmless may have unfortunate late consequences. It is possible that exposure to any amount of radiation produces some biologic effect, but serious acute radiation injury or death occurs only after exposure to relatively large doses.
Large-scale epidemiologic surveys in man indicate a linear relationship between dose and incidence of certain types of late radiation effects, e.g., certain radiation-induced neoplasms. Furthermore, the data give no indication of a threshold dose below which such damage does not occur. Although data in the very low dose range are admittedly meager, to be conservative one must assume that there is no threshold for certain types of somatic damage. Recent studies, however, indicate that radiation-induced damage to the DNA of cultured mammalian cells can be repaired and that mouse ova can recover from point mutations.
This allows us to hope that the linear relationship between radiation effects and dose may not hold in the very low dose range or at very low dose rates. The threshold concept does not apply to the acute radiation syndrome or acute localized injury. Such injuries occur only after the threshold dose has been exceeded.
Here You Will Know The Facts About Radiation Poisoning In Man And Radiation Sickness
Pathology
After total body exposure of animals to the usual doses responsible for the acute radiation syndrome, histologic examination reveals a prompt disappearance of mitotic figures. This is followed fry the gradual return of mitotic activity, some of the dividing cells showing obvious chromosomal abnormalities. Many of these injured cells, after an interval that tends to vary with the dose and the tissue, die following division or, in some instances, from giant cells before dying.
Primary radiation damage to blood-forming and intestinal tissues, i.e.. depletion of cells and temporary loss of ability of stem cells to repopulate the tissues, inevitably leads to secondary complications. Prominent among these is bacterial invasion with septicemia as a consequence of granulocytopenia, depressed immunology capabilities, and damage to the intestinal barrier. Infection and toxemia resulting from tissue breakdown lead to a pronounced inflammatory reaction in many tissues, particularly in the oropharynx and intestines, where extensive ulceration may occur.
The inflammatory reaction is distinctive in being almost devoid of granulocytes. Another complication is hemorrhage, varying from microscopic extravasation of erythrocytes to gross bleeding at the height of the illness. Late in the syndrome, epilation, particularly of the scalp, may be observed.
In acute localized radiation injury, both intermitotic and reproductive cell death occur, accompanied by a secondary inflammatory response. Upon recovery, endarterial thickening and extensive fibrosis develop gradually. In the case of late radiation effects, such as neoplastic disease, there may be no microscopic features indicative of prior radiation exposure.
Pathogenesis.
Although the total radiant energy dissipated in an irradiated cell is small, that involved in the interaction of radiation with individual molecules is sufficient to cause ionization and to break chemical bonds. The resultant chemical alteration of certain biologically important molecules, such as deoxyribonucleic acid (DNA) and chromosomal proteins is probably the basic lesion responsible for the so-called reproductive type of radiation death of cells. It has been calculated that exposure of a mammalian cell to one Roentgen of x-rays results in three single-strand breaks and three tenths of a double-strand cut in its DNA molecules.
This type of molecular damage may be compatible with life in nondividing cells, but may become evident when the cells recover from the temporary radiation-induced suppression of mitotic activity. The chromosomal aberrations seen in mitotic cells may result in an imbalance of genetic material in daughter cells that is incompatible with continued life and reproduction; such abnormal cells die after one or two mitosis. Rapidly proliferating tissues are radiosensitive in part because their widespread mitotic activity results in rather prompt death of the descendants of many cells with severe chromosomal abnormalities. In contrast to the reproductive death, the mechanism of intermitted cell death after massive exposure is poorly understood.
Clinical Manifestations.
The clinical manifestations of the acute radiation syndrome vary with the dose, and reflect damage to the three key organ systems, namely, bone marrow, intestine, and sometimes the central nervous system. With doses in the lethal range or below, the signs and symptoms are primarily those of marrow damage and secondarily of intestinal injury. With higher doses, the illness is more acute, and symptoms of severe intestinal damage overshadow those of marrow depletion. With very high doses, the clinical picture is one of acute central nervous system destruction with resultant disorientation, convulsions, hypotension progressing to shock, and fever. Skin erythema may appear promptly. Death occurs within hours or days before marrow and intestinal damage can significantly influence the manifestations.
Except in the fulminating central nervous system type of injury, the classic acute radiation syndrome can be divided into four phases. The first phase develops within minutes or hours after exposure and consists of nausea, vomiting, and, perhaps, diarrhea and weakness. A day or so later, symptoms subside, and the illness enters the second phase, a period of relative well-being. After an interval of one or more weeks, depending upon the severity of the illness, the third or critical phase occurs, primarily as a result of marrow failure and infection. Fever increases in a stepwise fashion, and vomiting and anorexia recur.
There may be stomatitis, which can progress to oropharyngeal ulceration. The abdomen may become distended, and there may be severe and sometimes bloody diarrhea. Petechial hemorrhages may be noted in the skin. The patient is obviously toxic, perhaps dehydrated, and shows evidence of marked weight loss. Epilation, particularly of the scalp, may occur during the third week. Death, primarily due to intestinal damage, may occur during the second week, before the period in which bleeding and septicemia develop. Following the critical phase, those patients who survive enter the fourth or recovery phase. Recovery almost inevitably begins before the sixth week, and convalescence is slow, residual weakness persisting for months. Temporary sterility may develop during convalescence, and cataracts may occur years later, particularly after neutron exposure.
Hematological data reflect damage to the radiosensitive blood-forming tissues. The lymphocyte count falls within a matter of hours, reaching a minimal value within four days. After exposure to large doses, lymphocytes may virtually disappear from the blood. An initial granulocytes lasting a day or so is followed by a fall in granulocytes, in severe cases reaching very low levels early in the second week. With less severe injury, the granulocytes count levels off about the eighth day, and may even show an abortive rise lasting up to 10 to 12 days. The count falls again during the critical phase of the illness, reaching a minimum during the fourth or fifth week in those patients who recover. In such patients, the platelet count begins to fall a few days after exposure, reaching a minimum at 28 to 32 days. The erythrocyte count falls gradually until the twenty-sixth to thirty-eighth day unless there is gross bleeding.
Other laboratory findings, none of which is pathognomonic of radiation injury, may be useful in evaluating severity of the illness. There is an increase in bleeding time during the thrombocytopenic period. Blood cultures during the critical phase may yield enteric bacteria. Analysis of the urine may show creatinuria and increased excretion of beta-aminoisobutyric acid, Maurine, and other amino acids and deoxycytidine. Following neutron irradiation, induced radioactivity may be detected in sodium and phosphorus of the plasma and in sulfur of the hair.
The clinical manifestations of localized irradiation depend upon the tissues involved.,In the skin, erythema develops within days or weeks after acute exposure, and may progress to epidermolysis. Following recovery, there may be atrophy of the skin with underlying fibrosis, telangiectasia, and eventual malignant degeneration. In radium poisoning, the first sign of injury may be a plastic anemia. Later, pathologic fractures and/or osteogenic sarcomas may develop. Similarly, malice# change can be the ultimate fate of almost heavily irradiated tissue
The late manifestations of whole-body exposure include life-shortening, acute or chronic myelocytic (not lymphocyte) leukemia and, possibly other myeloproliferative disorders. These illness do not differ from those that occur spontaneously.
Diagnosis.
Acute radiation injury is rare if a diagnostic problem. The history of excess radiation exposure is usually but not always obvious, particularly in persons occupational exposed. There have been instances of unsuspected occupational exposures and even unwitting exposure of an entire family. Therefore, the possibility of radiation injury should be entertainer in patients with aplastic anemia or pancytopenia of unknown origin, or other illness showing damage to blood-forming tissues.
With late manifestations of radiation injury the exposure history may be obscure. In the case of malignant conditions, perhaps the only reason for suspecting irradiation is the unusual age at onset, e.g., estrogenic sarcoma in an older person or acute leukemia or thyroid cancer in an adolescent. The. presence of internally deposited radioactive materials responsible for some late radiation effects can usually be demonstrated only by sophisticated hydrochemical or physical techniques.
Treatment.
Treatment of the acute radiation syndrome is symptomatic, directed at preventing and combating infection, controlling bleeding, replacing fluids and electrolytes and, when necessary, correcting anemia. Cronkite, Bond, and their associates, using the following regimen, have succeeded in sustaining life in dogs exposed tc supralethal doses of x-rays: (1) administration of broad-spectrum antimicrobial at onset of fever in the critical phase of the illness; as resistance to one antimicrobial developed, usually in three to five days, another was substituted; (2) fresh platelet or blood transfusions to stop bleeding: and (3) fluid and electrolyte replacement. Other symptoms, such as hypotension, shock, and pair.. should be treated systematically as they occur.
The current ideas about treatment of acute radiation injuries, including use of sterile hospital facilities, can be found in the article by Andrews and his associates. Bone marrow transplantation does not seem justifiable at present, except in those rare circumstances in which the patient’s own marrow had been stored prior to exposure or when marrow from an identical twin is available For patients who recover, a period of convalescence may be required and further occupational exposure should be avoided.
Treatment of localized forms of radiation injury is also symptomatic, for there is no way to undo or modify the injury once it has occurred. When certain bone-seeking, radioactive substances have been taken into the body, however, the possibility of injury can be reduced by administration of cheating agents, which increase their excretion rate.
Prognosis.
If a patient is known to have had of radiation, it is possible to predict with a fair degree of certainty the outcome of his illness. In the case of exposure in the lethal range, it is impossible to differentiate on the basis of dose alone between patients who will survive and those who will die. Limited information about dose response in man and individual variation in response restrict the value of radiation doses in predicting the course of the illness. In accidental exposures, there may be further uncertainty as to the actual dose and or exposure of the body. The prognosis of patients illness therefore must be based clinical grounds.
After careful analysis of all reported accidental exposures. Bond et al have classified the acute radiation syndrome into four categories according to the probability of recovery. In the first category, arrow virtually impossible, the estimated radial doses exceeded 500 to 600 rads (total-body exposure . In the second category, survival possible. the estimated dose range was 200 to 450 rads. In the third, survival probable, the range was ICO to 200 rads. Exposures in the fourth category, survival virtually certain, were less than 100 rads. The patients in category I have severe central nervous system damage or predominantly intestinal symptoms.
Their blood studies showed severe depression of all formed elements by the second week of the illness. The patients whose survival was considered virtually certain (category IV) had mild symptoms, if any, and no evidence of severe marrow damage.
The patients in the survival possible II; or survival probable (III) categories could not be differentiated early in the illness, although lymphocyte counts below 1000 to 1200 cells per cubic millimeter,’severe diarrhea, and skin erythema were .ominous signs. Even in the critical phase it was difficult to be certain whether the patient would live. Once the marrow began to recover, usually not later than the fifth week, survival was almost certain. Except for an increased chance of developing late manifestations of exposure. recovery from the illness was virtually complete in all survivors.The prognosis for localized injuries can be found :u radiation therapy textbooks; that for late manifestations is the same as in the spontaneously occurring diseases.
Prevention.
Occupational radiation injury is minimized and largely prevented by rigorous enforcement of strict operating regulations. These procedures are designed to avoid accidental overexposure and to limit unavoidable exposure to radiation levels that are not believed to cause detectable bodily damage. .
Because medical roentgenologic procedures are responsible for the major share of the total exposure of our population, it is the duty of every physician to keep patient exposures to the minimum compatible with good medical practice. As mentioned earlier, the risk to any individual is so small that patients should not be denied rent geographic examinations that could be beneficial.
The physician must weigh the risks against the possible benefits in each case. Radiation therapy of benign disease in persons with long life expectancy should be avoided in favor of other forms of treatment. Since the fetus is radiosensitive, particularly during the first eight weeks of gestation, abdominal exposure should be avoided in pregnant women if possible. Some experts recommend that elective abdominal fluoroscopy of women of childbearing age should be done only during the first two weeks after menstruation to avoid irradiation of unsuspected fetuses.